tick map Canada
map by Ontario Animal Health Network
If you’d asked me a few years ago, I wouldn’t have said that’s a question I’d expect to get (daily). However, we’re in a different world tick-wise now, so it’s a common and understandable question, particularly because of our tick tracking efforts (for Canadians).
The answer is no/possibly/maybe later.
How’s that for a straight answer?
We are not testing all ticks that we get through tick tracker submissions, but we will be testing some for specific reasons not related to patient health. It’s important to understand why we don’t test for the sake of the patient.
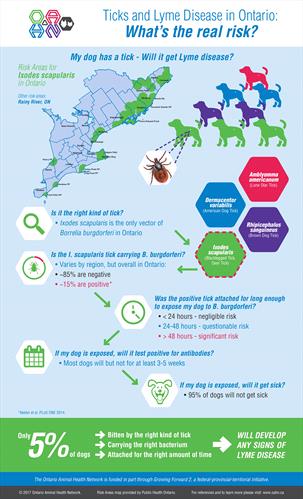
For a dog (or person) to get Lyme disease, several things all have to happen:
- It has to be bitten by a tick.
- The tick has to be a species that carries B. burgdorferi, the bacterium that causes Lyme disease.
- The tick has to actually be infected with the bacterium.
- The tick has to be attached long enough to transmit the bacterium during feeding.
- The bacterium has to escape the immune system and cause an infection.
We cover #1 and #2 with our tick tracking. If the tick isn’t a black legged tick, then Lyme disease isn’t an issue (and testing the tick for that bacterium makes no sense).
If it is a black legged tick, does testing of the tick help?
Not too much.
A positive test from a tick means that the tick carried the bacterium. It still had to be transmitted to the bitten individual and it had to escape the individual’s host defenses. That obviously happens in some cases, but in dogs, it’s estimated that Lyme disease occurs 5 percent of the time, or less, when an infected tick has been attached long enough.
A negative test means the tick was probably negative. However, if the dog was exposed to one tick that was tested, it’s reasonable to assume that there may have been undetected ticks too.
The most important things are:
- Was it the right tick species?
- Is Lyme disease endemic or emerging in the area where the dog picked up the tick?
- Was the tick attached long enough to transmit B. burgdorferi if it was infected?
If the answer is yes to all of these, then there’s risk. Testing the tick provides more information, but it doesn’t change what we do. Post-exposure prophylaxis is something that is done in people in certain circumstances, particularly when the answer to the three questions above is “yes” AND the tick was removed within the past few days. Tick testing isn’t necessarily that quick, dogs are less likely to develop disease than people after exposure and we have no evidence regarding whether prophylaxis is useful in dogs.
So, my approach to finding a tick, from a clinical standpoint, is to:
- Emphasize the need for good tick prevention in the dog
- Emphasize the need for Lyme disease awareness
Testing doesn’t change what I do to manage a canine patient. However, it can be useful from a research standpoint to let us know about infection rates, what other pathogens might be present, the strains of Borrelia that might be involved, and similar (often poorly investigated) areas).
Tick testing is available commercially but I don’t recommend it because it doesn’t change what I do.
If the tick was positive, I’d say “you need to do good tick prevention” and “you should be aware of Lyme disease” and “we need to consider Lyme disease if your dog develops signs that could be consistent with that disease.”
If the tick was negative, I’d say “that tick was negative, but what about any others?” Then I’d say “you need to do good tick prevention” and “you should be aware of Lyme disease” and “we need to consider Lyme disease if your dog develops signs that could be consistent with that disease.”
Since it’s the same answer in either case, there’s not a lot of use for routine testing, from my standpoint.
So, keep the tick reports coming to our tracking site at PetsandTicks.com and feel free to send any to us for identification (as described through that site). However, don’t expect routine testing for Borrelia since it won’t change what we recommend for your dog.
Reprinted with permission from Worms and Germs Blog.