Hypoglycemic kitten Cracker Barrel syrup
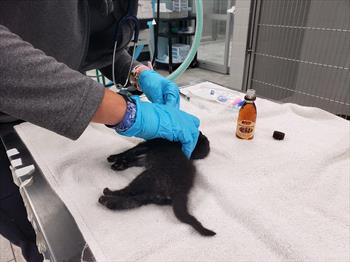
The tiny bottle of life-saving syrup is next to the kitten. Photo by Dr. Tony Johnson.
Sometimes, you have to get creative.
When teaching new-grad doctors and veterinary students, I often espouse the benefits of remembering the ABCs – Airway, Breathing and Circulation.
If this sounds familiar, these are the first steps in CPR. It’s how I deal with a new patient in the veterinary ER where I work, and a good way to avoid the adrenaline rush and subsequent discombobulation that happens when a hot emergency gets wheeled in.
I’ve been doing emergency work for 25 years and I still get butterflies when something big comes into the room and lands in my lap. The ABCs help me regain control and prioritize what I have to do to give the patient a chance. It keeps me grounded and functional in the face of panic.
In human pediatric medicine, however, they amend the ABCs just a bit to the ABCS – and that last “S” that got promoted from a wee signifier of pluralism to a capital S stands for sugar: little patients, of both the human and animal variety, tend to get hypoglycemic quickly and adding that big S into the algorithm for resuscitation helps them remember to check a blood glucose early in the process when dealing with a sick child, kitten, or puppy.
No sooner had I begun bloviating about the ABCS to a couple of new ER docs when a tiny kitten was rushed in. The poor thing was flat out, hypothermic, and not looking very good at all.
Any puppy or kitten who comes into the ER is hypoglycemic until proven otherwise (with a glucometer, just like people use). As we get our supplies lined up and look for a tiny vein for a blood sample to check blood glucose we often rub dextrose solution on their gums – dextrose is a form of sugar. The hope is that they will absorb a bit of it across their gums to help bring their blood glucose up until we can check the level and give some IV.
So, this tiny kitten needed some dextrose. The problem was we didn’t have any.
For some reason, the bottle of dextrose was nowhere to be found. It’s cheap stuff (basically sugar water) and I’d bet that just about every veterinary hospital from Poughkeepsie to Pretoria has a bottle lying about.
Except mine.
After the short, frantic search for the dextrose, I remembered that the hospital had catered a breakfast for the staff that day from Cracker Barrel, and that always came with scads of wee adorable bottles of their pancake syrup. I had one sitting in the office with the intention of taking it home. (My son loves them. I remember him saying once when he was about four: “Oh! Tiny syrup!”)
I dashed into the office and cracked the seal on the bottle. My technician looked at me as if to say, “Now’s not the time for pancakes, chubby!” but got the idea when I asked her to rub some on the poor kitten’s gums.
When the sugar buzz hit, the little kitten held her head up a bit a let out a tiny meow. The Cracker Barrel trick had worked! It had bought us enough time to get an IV catheter in place and give some fluids. Once she was a little more alert, she got some wet food (with more syrupy goodness mixed in) and felt much better. Turns out, a common GI bug called coccidia had laid her low, she stopped eating and everything went downhill from there until we hit her with the Cracker Barrel Treatment.
If you have a small dog, like a Yorkie or toy poodle, they can be any age and prone to hypoglycemia if they stop eating. And if you have a kitten or puppy who isn’t eating (it can be as little as a few hours), they can be at risk for low blood sugar. If you notice they are looking droopy or acting lethargic, try to get them to eat (if they aren’t vomiting). If they eat – great. Time to head to the vet.
But, if they don’t or won’t or can’t eat and are laid low like our little friend here – good old pancake syrup rubbed on the gums can be a lifesaver while you’re on your way to your vet or the veterinary ER.
It doesn’t have to be Cracker Barrel brand, but I now have proof that it works in a clinical setting. The buttermilk pancakes aren’t quite as useful, so we ate all of those.