CPR in hospital Fletcher
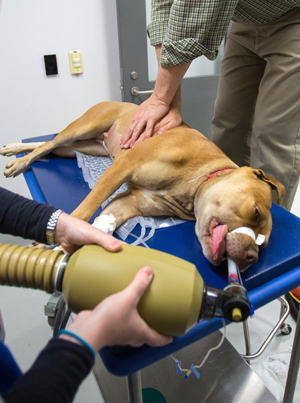
Photo courtesy of Daniel Fletcher, PhD, DVM, DACVECC
Sometimes the unthinkable happens, and if it’s your pet you’d want the medical team caring for them to be prepared for it. You’d also want them to know your wishes and act accordingly. One basic fact that you need to know: CPR in pets isn’t like CPR on TV (or even CPR for people in the real world). On TV and in movies, CPR works about 80 percent of the time. The victim pops up, shakes their head and seems fine two minutes after they were going towards the light. In the real world: not so.
For people, the success rate of CPR in real life varies with whether it happens in the hospital or on the street, and also it depends on how long it takes first-responders to get to you, but it’s safe to say that it’s nowhere near the success rate on TV.
The rate of pets miraculously coming back to life after their heart stops and breathing ceases is even more miniscule; it’s about 10 percent or less. It varies, again with medical condition and species (cats fare slightly better than dogs), but it’s a small percentage. When discussing this topic with owners, my standard blanket statement (unless anesthesia is involved – more on that in a bit) is that the success rate of CPR in getting animals home and functional is in the low single-digits. It’s that bad.
There’s one other big distinction in terms of the success rate of CPR and that’s whether it happens due to an illness or trauma (which is most cases), or whether it happens under anesthesia. If a patient has a cardiac arrest under anesthesia (which is thankfully very rare, far less than one percent of procedures, due to today’s safer anesthetic practices), those patients have a far better chance of going home. The otherwise healthy dog or cat who has a cardiac arrest during a spay operation has a much brighter chance of making it home than does a 19-year-old cat dying of kidney failure or cancer in ICU.
We tend to want to hold on to our pets because we love them, but sometimes that love runs right into a hard brick wall of reality that we wish didn’t exist. One of those bricks is that if a pet has a cardiac arrest because of a serious illness, that death may be a normal part of life. It feels a bit like heresy to say that, since as a doctor we’re trained to battle death and illness, but acceptance of death as natural is becoming more widespread in both the human and veterinary medical fields (Atul Gawande’s excellent book "Being Mortal" is an eloquent treatment of this complex and nuanced topic).
I think it’s high time that this acceptance of death extended to the general public. Our faith in medicine as curative for illness should not extend to natural death, which in some circumstances we should welcome. Knowing when a death is natural or premature will always be the gremlin in this decision-making process, and it will be eternally imperfect and we will question it – which means we’re grappling with the big questions, which means we’re getting it partially right. That’s close to good enough for me.
I’m not saying we shouldn’t try and fix bodies that are ill, as that’s the whole purpose of veterinary (and human) medicine, but we do need to take ownership of two concepts. One: We can’t fix every problem that exists, and Two: death is a natural part of life.
One of the things that I often discuss with pet owners when I’m admitting patients to the hospital for a serious illness like cancer, systemic infection, or organ failure is what they’d like me to do in the event of a cardiac arrest. Believe me, it’s an uncomfortable conversation in many cases, and one I’d rather not have. But it’s a vital one. If I guess what an owner wants rather than asking, there’s a real risk that I’ll guess wrong and try CPR on that 19-year-old cat, with its attendant indignities and expense, or (perhaps worse) not do CPR on that 6-month-old dog whose heart stopped while I was spaying her. In both cases, I haven’t helped man or beast.
That’s why we ask and endure that oftentimes uncomfortable conversation with the questions and statements that occasionally come up like “Well, if she’s going to die in surgery, I’m not going to spay her,” or “So, you’re saying he’s going to die?”
I won’t lie – it’s easier not to ask. It’s not fun, and sometimes is devolves into a 30-minute conversation, which in the ER is sometimes something of a luxury. But it needs to be done, and like flossing and eating broccoli, I make myself do it. Talking about this has saved me, and saved my patients, countless times. Saved lives, and saved me and my staff from making the wrong call.
Sometimes just broaching this taboo topic makes people think that this is my passive, backhanded way of saying I think their pet won’t make it. It’s not. It’s just me being thorough, but it’s such a scary topic that to many people it’s like that old game of Bloody Mary; if we’re talking about death, it might just show up.
One option, and one that I will unabashedly discuss with owners and sometimes present as perhaps the best option is the DNR (Do Not Resuscitate) order. This means that if breathing or heartbeat stops, we don’t intervene: no breathing tubes, no drugs to aid circulation, no chest compressions. We do nothing but notify the pet owner and provide pain medication and possible aid in dying if the owner consents. There is some gray area here, as sometimes a patient will stop breathing, lose consciousness, and then linger on in a biological gray zone, sometimes for hours. For these cases, we will discuss hastening the dying process, but this is a discussion that takes quite a bit of caring and finesse. (In most cases, it’s thankfully a little more clear-cut and patients avoid the gray zone and pick life or death rather quickly.)
Needing to know what the owner wants guides our hand in how we intervene with the patient. But in order to know, we have to ask, we have to listen, and we have to communicate with members of the team giving care to the patients. Most of the time, there’s a bright pink DNR or red CPR sticker at the top of the medical chart hanging on a patient’s cage so everyone knows what to do; the DNR one looks remarkably like the “Thank You” stickers that my kids always ask for at the grocery store.
There should be no shame in choosing DNR orders, either for yourself or for your pet. There’s also nothing wrong with going guns blazing and doing rock-solid perfect CPR when the conditions are right. Experience and training are what help us decide when and who to try and resuscitate. But many owners beat themselves up because they “didn’t try enough” when choosing a DNR, as if they’ve failed their pet somehow. In my experience, the risks of doing too much with modern medicine far outweigh the small risk of not doing enough in most cases. The modern phenomenon of dying alone in ICU at 3 a.m. with tubes in every natural orifice and a few medically created ones is no way to go, regardless of whether you are human, dog, or cat.
A lot of owners feel shame when picking the DNR option. Perhaps if they knew the minuscule odds of coming home to a normal life, they’d start to feel some of the acceptance, with a hint of peace, that I do when I know a patient has lived a good life, and was given the final dignity of being helped to experience a good and natural death.
3 Comments
Ariana
August 23, 2016
Cat Tayler
August 21, 2016
Ann Wortinger
August 19, 2016