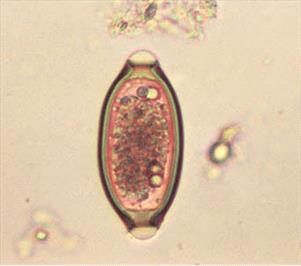
Photo courtesy of CDC / B.G. Partin
This micrograph depicts an egg from the “human whipworm,” Trichuris trichiura.
Veterinarians love excrement. As a group we’re obsessed with it and often have to be reminded that “The horse in stall 2 pooped today!” is not a great opener to dinner conversation. Bowel movements are diagnostic treasure troves. Poop can tell us how well an animal is eating or drinking, what it ate, whether it’s experiencing a GI bleed, and what critters inhabit the mammalian mother ship – possibly parasites.
A parasite is a small organism that lives at the expense of a large host organism: Much like children, but without the winsome smiles.
Parasites come in multiple shapes and sizes and affect different organ systems in the host, playing havoc with everything from the skin to the GI tract, and even heart and lungs; think of roundworms and heartworms. Despite their differences, mammalian parasites share some similarities. Generally, these critters have a multi-stage life cycle that depends on infected animals shedding some stage of the parasite in some form of bodily goop – blood, urine, or our topic of the day, feces. In order for the parasite to continue its domination of the planet, new animals must come into contact with the infective form of the parasite. In the case of GI (poop)-inhabiting parasites, this contact occurs when the vulnerable animal’s food becomes contaminated with the feces from an infected animal.
In most cases cattle, horses, sheep, and goats no longer range freely, moving off of contaminated forage as they go. Instead, they are frequently confined to relatively small pastures where parasite-containing fecal material (poop) mingles with the forage. Dogs and cats have moved from the barn and yard to the living room and bed. Parasites and their hosts no longer cohabitate harmoniously.
For grazing animals, the proximity of bathroom and kitchen makes the GI parasite’s job an easy one. Horse A is infected with roundworms. Horse A poops on grass. Horse B eats grass and with the grass, the parasite larvae that have crawled up the juicy stems from the steaming pile of you-know-what. Horse B becomes infected with roundworms. Maybe.
Did you catch that last bit?
Just like not everyone is allergic to shellfish or can carry a tune, not all animals are equally susceptible to parasites. Age, immune function, and possibly genetics determine which animals are more likely to become infected.
Parasites can cause lots of trouble, but the degree of parasite mayhem is dependent on the level of exposure and the susceptibility of the animal. For instance, stick a puppy in a kennel full of whipworm-laden littermates and the poor little guy will be infested before he can blink twice. Conversely, an adult horse’s immune system is likely to laugh at a pile of manure-containing roundworm larvae in one 10-acre pasture.
A timeline of parasite control would show a shift from “that’s just the way it is” to genetic selection of parasite-resistant animals and reduction of fecal contamination of pastures (picking up the poop), to labor intensive and rather toxic chemical drenches, to today’s safe, effective, and convenient drugs used for deworming.
When the modern classes of anti-parasitic drugs appeared in the 1980s, they seemed almost like a magic bullet. These drugs came in pastes, shots, pills, and even in chewable treats. They killed a wider array of parasites than any drench or potion before, and – even better – they were unlikely to kill the patient. This was exciting stuff!
Veterinarians, ranchers, and pet owners alike embraced the wonder drugs and adopted a parasite vigilante position. No worm shall escape our wrath!
Except some did.
Just like not every animal is equally susceptible to parasites, not every parasite is equally susceptible to drugs. Over time, some parasites have escaped the deworming onslaught, and crept off “underground” like Morlocks to breed and plot their return. The offspring of these more resistant parasites carry the same decreased vulnerability to drugs as their parents, they breed, and before you know it, suddenly people wonder what happened to the wonder drugs.
As with gluten-free Oreos, it is dangerous to embrace the wonders of deworming willy-nilly and caution-free. When we stopped managing manure and began throwing anti-parasitic drugs at everything on four feet, we started messing with Mother Nature, and she is one pissy lady when you don’t check in with her first.
It turns out that routinely deworming everything on four legs is a fast way to spend a lot of money and create some tough-as-nails parasites.
Just as jeggings are not one-size-fits-all, a cookie cutter approach to deworming isn’t the best fit. When I started in equine practice, the common deworming routine involved rotating deworming drugs every 6-8 weeks for every horse, no matter what. We were operating from the best information we had. But over time, strange things started happening. Foals from “well-managed” farms were becoming sick with huge parasite loads. They shouldn’t have been, but they were.
It turns out that something like 20% of horses are responsible for shedding 80% of parasites. This means that by deworming every horse in the same way, we were:
- Over-treating 80% of the horses
- Under-treating 20%
- Selecting for resistant parasite populations.
If you have horses, you may have noticed your vet recommending annual or bi-annual fecal exams more often or something called a Fecal Egg Count Reduction Test (FECRT). The idea here is to identify the horses that need to be dewormed and to treat them, not all of the horses. At the same time, this testing can help identify what drugs work best on which farms.
For dogs and cats, the parasite-control world is a little different. Horses don’t sleep in human beds. Children don’t play in horse pastures nearly as often as they play in parks or yards where dogs and cats have been. While most horse parasites ignore humans, the same can’t be said for the critters that call dogs and cats a host.
Parasites of dogs and cats can cause all sorts of nasty human symptoms from skin problems to blindness. Since dogs and cats share our blankets, a blanket approach is exactly what is used to keep their parasites at bay.
However, resistance is still a potential problem in the pet world as well as the large animal one.
What to do? Use of anti-parasitic drugs contributes to resistance, but parasites make humans and animals sick. Is the sky falling?
Hold up, Chicken Little. The sky is still hanging in there. We are not doomed to become subjects to parasite overlords anytime soon. But it’s a good idea to take a look at how we live with these critters:
- Find out what your veterinarian thinks is the most sensible approach to parasite control given your location and the members (two and four legged) of your family.
- Make sure that when you give anti-parasitic meds, the entire dose goes in the animal.
- Pick up the poop. In the pasture, stall, back yard, community park, dog park, or litter box, do your part to break the parasite life-cycle by managing the manure.
- Wash, wash, wash. Hand washing is still and always the best way to keep humans healthy.
We may not be able to get rid of the parasites, but we can manage them more effectively than we used to – and that’s best for our own health as well as that of our animals.