Lymphoma is currently the most common malignancy in cats, accounting for as much as 30 percent of all feline cancers. Luckily, it is just as responsive to medication as it is in dogs, and prolonged remissions are common. This article reviews the common forms of lymphoma in cats, including diagnosis and treatment expectations.
Lymphoma is a cancer made of lymphocytes, and these lymphocytes readily travel throughout the body via the lymph system. Because of all this traveling, lymphoma is only a localized problem in rare situations, so surgery and radiotherapy are not appropriate as sole treatments. To reach cancerous lymphocytes in all the places they have gone, medication (chemotherapy) is necessary because medication can be carried all over the body via circulation. Treatment of lymphoma is going to involve pills and/or injections for your cat, regardless of which form of lymphoma has been diagnosed.
Classification by Anatomical Location
As in the dog, one of the more common ways to classify lymphoma is by the anatomical area (meaning location on the body) where the cancer is mainly located.
In dogs, the most common form of lymphoma is the multicentric form, where many (if not all) of the body’s lymph nodes seem to enlarge and fill with cancer cells at the same time. Cats are certainly able to develop multicentric lymphoma as well, but by far, the most common form of lymphoma in cats is the intestinal form, so most of this discussion will center there. Other notable forms of feline lymphoma include renal (kidney) lymphoma, nasal lymphoma, and mediastinal lymphoma.
Intestinal Lymphoma
As mentioned earlier, lymphoma can develop anywhere there is lymph tissue, and virtually all organs have some bits of scattered lymph tissue associated with them. It is unclear why some areas seem especially vulnerable to developing lymphoma over others.

Illustration courtesy Dr. Wendy Brooks
In the past, the feline leukemia virus was the chief cause of feline lymphoma development. Until there was a feline leukemia virus vaccine, the intestinal form of lymphoma was unusual. Now that Felv vaccination is common, intestinal lymphoma accounts for 50-70% of all cases of feline lymphoma.
Cats with intestinal lymphoma tend to be seniors (ages nine to 13 years on average) with a chronic history of weight loss, vomiting, diarrhea, or all three. Appetite is variable, which means it may be normal, excessive, reduced, or non-existent.
Intestinal lymphoma may be a distinct mass or growth or group of growths, or appear as a more subtle infiltration of cancerous lymphocytes into the delicate membranes of the bowel lining. Infiltrative lesions, which are often invisible to the naked eye, generally respond to chemotherapy; surgery is not necessary or even helpful. Distinct masses, however, can cause an acute obstruction and may require surgical removal to relieve this potential emergency. Removing these masses does not control the cancer, and chemotherapy is still needed after the surgical site has healed.
Diagnosis
Confirming lymphoma requires a sample of tissue, ideally a small chunk or at least a smear of cells. There are several ways to harvest tissue for analysis.
Surgical Biopsy
Surgical biopsy involves opening the abdomen and removing pieces of tissue for analysis.
- Pros: Maximum access to the abdomen's organs, ability to sample the full thickness of the intestine, and see how deeply the abnormal cells penetrate. This type of sample not only distinguishes benign versus malignant disease but also allows for grading the lymphoma, which is important in prognosis (see below).
- The cons are that it is invasive and requires general anesthesia and hospitalization. Also, chemotherapy must be delayed until the surgery site has healed.
Endoscopic Biopsy
Involves the use of a long scope inserted into the mouth and/or anus to view the intestine and stomach from the inside. A small “biter” is inserted through the scope that can bite out little pinches of intestinal tissue; these biopsies are not full thickness, but the scope allows for specific areas to be sampled.
- Pros: Far less invasive than surgical exploration, with patients generally going home the same day as the procedure. A quality biopsy, as mentioned, distinguishes benign versus malignant disease and allows for grading. Chemotherapy need not be delayed after results are obtained. Areas that might not look abnormal when viewed externally may look very abnormal when viewed from inside the intestine, and endoscopy allows for any such specific areas to be biopsied.
- Cons: Does not always produce quality samples as readily as surgery. Endoscopic samples are smaller, not full thickness, and may be squashed by the biopsy biter, making interpretation more difficult. Also, only the intestine is accessible; other organs are not. Requires general anesthesia (though usually not hospitalization).
Needle Aspiration
Involves removing a sample of cells from a larger organ or from a mass with a needle, usually with ultrasound guidance.
- Pros: Anesthesia is rarely needed, and the procedure is less invasive than the other two methods.
- Cons: Cells are withdrawn without their tissue architecture, which means some accuracy is sacrificed. Non-diagnostic samples are not unusual. The intestine itself cannot be aspirated; only masses and organs (local lymph nodes, the liver, etc.)

Ultrasonographer imaging an animal patient. Photo courtesy of DVMSound.
Ultrasound without Biopsy?
Ultrasound represents a non-invasive means to evaluate the texture of the organs of the abdomen. Intestinal lymphoma tends to have a characteristic disruption of the bowel lining that is visible by ultrasound. Further, lymph node enlargement in the abdomen can be evaluated, as well as texture in the liver. Lymphoma can be quite subtle in its manifestation, but if the appearance of the bowel on ultrasound is classical, it may be reasonable to begin treatment based solely on this information and forego the more expensive/invasive biopsy procedures. Learn more information on infiltrative bowel disease and the pros and cons of treating it without tissue sampling.
Another way that ultrasound might negate the need for further procedures is by obtaining a diagnostic aspirate. If there is a mass or if the local lymph nodes are enlarged, they may be aspirated as described above. If the cells obtained indicate that lymphoma is present, then the diagnosis has been adequately obtained.
Furthermore, the appearance of the intestine and lymph nodes is often ambiguous. In this situation, the liver can be aspirated despite its normal appearance. Often, lymphoma can be found hiding out there. Again, if a diagnostic aspirate is obtained via ultrasound, it is unnecessary to pursue surgery or endoscopy.
High-Grade VS Low-Grade
One of the advantages of having an actual tissue sample is the ability to grade the malignancy of the lymphoma. Lymphoma is graded by the pathologist, who reads the biopsy sample as high-grade, low-grade, or intermediate-grade. The grade refers to how rapidly the cells appear to be dividing and how malignant they appear, with a high grade being the most malignant. The grade of lymphoma bears on its response to chemotherapy (see below). It may be possible to grade a lymphoma with an aspirate sample, but it is vastly easier with an actual chunk of tumor. As a general rule, with lymphoma, higher grades tend to be more responsive to chemotherapy drugs. With feline intestinal lymphoma, however, it is the low-grade cases that achieve remission more easily and for prolonged periods.
Treatment
As with most forms of lymphoma, treatment centers on medication rather than surgery or radiation therapy. The use of medication to treat this disease is called chemotherapy, a term fraught with unpleasant connotations. It is important to realize that cats rarely experience nausea, poor appetite, or malaise with their chemotherapy, and you should not make decisions thinking the cat will be put through some difficult procedure. Instead, the difficulty centers not around side effects but around giving daily medication to a cat and regularly bringing the cat to the veterinarian's office for injectable treatments and monitoring tests.
High-grade (also called lymphoblastic) lymphoma is bad news. Only 25-50% of cats achieve remission, and those that achieve it generally sustain it for only two to nine months.
Fortunately, most feline lymphoma is a low-grade (also called lymphocytic) form of lymphoma. This form behaves much more like inflammatory bowel disease, and treatment for severe IBD is largely the same as for low-grade intestinal lymphoma. Approximately 70% of cats with this form of lymphoma will achieve remission, and the median survival time is 23-30 months. Treatment for this form of lymphoma generally involves oral medication: prednisolone and chlorambucil. Many people opt to treat with these two medications based on the ultrasound appearance of the GI tract, playing the odds that there will be a response. Given the expense of more accurate diagnostics, this may be a reasonable alternative approach.
Ultrasound of a Kidney with Lymphoma
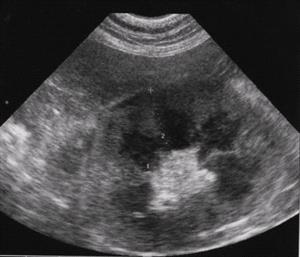
Photo Courtesy Dr. Ginny Kunch
Renal Lymphoma
Renal lymphoma is lymphoma in the kidneys and is one of the worst forms of lymphoma for a cat to contend with. In most cases, the cat is brought to the veterinarian for symptoms related to insufficient kidney function: poor appetite, excessive water consumption, weight loss, and possibly vomiting. Unlike the more typical cases of kidney insufficiency, where the kidneys are shrunken and small, the cat with renal lymphoma will have symmetrically large kidneys. A needle aspirate of the kidney usually reveals lymphoma cells.
With chemotherapy, kidney enlargement reduces, and often, kidney function improves until remission is lost. Median survival is only three to six months, though a recent case report highlighted a cat who lived many years, so long remission times are not impossible. Approximately 50 percent of cats with renal lymphoma are also positive for the feline leukemia virus, which carries the potential for other complicating issues.
Unlike other forms of lymphoma, renal lymphoma is strongly associated with tumor spread to the nervous system (brain or spinal cord). This makes for an unpleasant complication, and, unfortunately, this occurs in up to 40 percent of renal lymphoma cats.
Mediastinal Lymphoma
The mediastinum is not a structure with which most people are familiar. Most people know the chest cavity contains the heart, lungs, and other affiliated structures. But these organs are not just loose and flopping around in the chest; they are not simply held in place by gravity. The mediastinum is a sheet of connective tissue that bisects the chest and contains the heart, esophagus, trachea, and other central structures similar to a vacuum-packed plastic bag. The mediastinum divides the chest into right and left halves and stabilizes the location of the organs in the middle.
The thymus gland (generally atrophied in adult animals) and the mediastinal lymph nodes are involved in lymphoma. These are lymph system tissues that become the seat of mediastinal lymphoma.
When these lymph structures fill with lymphoma, the normal fluid drainage of the chest is hampered, and fluid begins to back up in the chest, creating a pleural effusion. This fluid takes up space in the chest that would normally go to expanding the lungs, and when the lungs cannot expand, the patient cannot breathe. Shallow, rapid breaths, possibly with the mouth open, result in the patient focusing on breathing rather than normal activities, including eating. The fluid can be tapped off the chest using a needle, and a sample can be sent to the laboratory for analysis. Usually, lymphoma cells can be found in the fluid if the cat has mediastinal lymphoma. Treatment is chemotherapy, as with the other forms of lymphoma.
Most mediastinal patients are young (less than five years old) adults, and most (80%) are feline leukemia virus-positive. Siamese cats seem to be predisposed to this form of lymphoma. In the days before the vaccine for the feline leukemia virus, mediastinal lymphoma was the most common form of feline lymphoma. It is rarely seen today. Cats that are positive for the leukemia virus tend not to live as long because of other complications. Still, remission is readily obtained regardless of the viral infection in most cats.
Nasal Lymphoma
Although nasal lymphoma is rare, it bears mentioning because it is the only form potentially localized to one area. Cats with nasal lymphoma typically have nasal swelling, sneezing, and nasal discharge.
Localized disease (e.g., the tumor in the nose) can be treated with radiotherapy or chemotherapy. In general, as with other forms of lymphoma, the disease is assumed to have traveled to other (distant) areas of the body. Because distant disease is addressed with chemotherapy, and it is assumed that lymphoma patients have distant disease along with their local disease, most nasal lymphoma patients receive chemotherapy.
Prolonged remission times (median survival times over 500 days) are possible with treatment.