Also called vaccine-associated fibrosarcoma and vaxosarcoma.
Back in the 1990s, researchers began to take note of locally aggressive tumors developing in the feline scruff of the neck, where vaccinations and therapeutic injections were typically given. The idea that vaccination (and potentially other types of injections) might occasionally cause cancer began to circulate in the feline medical community. By 1997, a task force was assembled to study the situation and make recommendations. We have come a long way since this time. What should you know about the feline injection site sarcoma (FISS) situation?
What Is an Injection Site Sarcoma and Why Do We Think Vaccination Might Cause it?
Soft tissue sarcomas have been recognized as difficult, deeply rooted tumors in cats for a long time, long before injections were ever involved. There are many types of soft tissue sarcomas, with fibrosarcoma being one of the most common. The fibrosarcoma is a tumor that does not usually spread throughout the body in the way we usually think of cancer; instead, it digs in deeply and widely in a localized area. After surgical removal, it is notorious for recurring even more aggressively than before. Distant spread does occur but much later in the course of the disease.
How a Fairly Small Lump can Invade Deeply

How a Fairly Small Lump can Invade Deeply. Image Courtesy MarVistaVet.
Fibrosarcomas have been recognized for a very long time, but the potential for vaccination to lead to the formation of a fibrosarcoma is a relatively new concern. The idea that cats could develop a sarcoma associated with vaccination began to receive attention when some of the following facts emerged:
- When local laws in a geographic area change to require rabies vaccination for cats, the incidence of fibrosarcoma increases in that area.
- Hawaiian cats have a reduced incidence of fibrosarcoma (rabies vaccination is not generally done in Hawaii as the islands have successfully eradicated rabies).
- The most common sites for these new, especially deep fibrosarcomas are the area between the shoulder, the lower back, and the hind limb (areas commonly used for vaccination).
- Some of these tumors contained vaccine adjuvant (material needed to boost the effectiveness of killed virus vaccines).
- Dogs are so rarely affected by this phenomenon that is considered of no realistic significance for them. Vaccine-induced fibrosarcomas seem to be a feline problem only.
Reports of sarcomas stemming from other injections followed, and it is now accepted that chronic inflammation concentrated in a small area is the root of the feline injection site sarcoma. Killed virus vaccine especially creates the exact scenario that can create sarcoma in an individual with the right predisposition for it.
Despite the extremely low incidence of this problem, the problem is still serious, and the veterinary profession has responded with numerous studies on how vaccines might be related to tumor formation, why the incidence is so low given how many vaccines are given to cats annually, and what can be done for prevention.
The vaccination uses a modified version of the virus to stimulate the immune system against the natural infectious virus. The modified virus can be alive but weakened, or it can be killed. (Recombinant vaccines are a story for another time.) A modified live virus will circulate through the body in a natural way typical of the infectious virus. As it moves through the body, it stimulates the immune response but doesn't generate illness.
A killed virus vaccine presents the virus to the immune system, but the virus is dead and doesn't replicate, bind anywhere, or do anything that a live virus might do to stimulate immunity. In fact, the body will tend to clear out the dead virus as it clears out other microscopic debris, and if this happens too quickly, a quality immune stimulation will not result. To see that this does not happen, adjuvants are added to hold the dead virus in place and attract the attention of the immune system. This kind of stimulation can lead to localized inflammation in the vaccination area; one theory is that this inflammation is what leads to precancerous changes in the local cells. Indeed, some fibrosarcomas have been found to have vaccine adjuvants embedded within them.
Every manufacturer of killed virus vaccines (which in cats are typically rabies vaccine and feline leukemia vaccine) makes its own adjuvant, and no single adjuvant has been implicated in the sarcoma phenomenon. Current thinking is that the cat's genetic makeup is just as important in determining if this kind of inflammation can lead to a pre-cancerous change in the tissue. Most cats do not generate cancer from localized inflammation: it takes the "right" cat and the "right" vaccine.

Image Courtesy of MarVistaVet
How Often Does This Happen?
Happily, not very often. Sarcoma incidence is extremely rare, with different studies reporting an incidence between one in 1000 to one in 10,000 vaccines given. To put this in perspective, using the traditional vaccination guidelines a cat would receive three vaccines annually during their 15-year lifespan for a total of 45 vaccines, not including the initial kitten series. In other words, a typical cat would receive 45 vaccines in its lifetime, and a sarcoma erupts in 1000-10,000 vaccines. Now that we have some prevention strategies, the incidence is likely to be even less.

Image Courtesy of Teri Ann Oursler, DVM
It can take as short a time as two months and as long as 10 years to develop a vaccine site tumor, but most appear within four years of the offending injection. While most (80 percent) of the tumors that develop are fibrosarcomas, other types of tumors that can develop through this phenomenon include:
- the malignant fibrous histiocytoma
- the osteosarcoma
- the rhabdomyosarcoma
- the liposarcoma
- the chondrosarcoma
- the undifferentiated sarcoma.
All are tumors of muscle, bone, cartilage, or fat.
Should I Still Vaccinate My Cat? What Has Been Done about this Problem?
Vaccination remains one of the most important aspects of preventive care for cats, and the risk of tumor development was already low before new policies were developed to make it even lower. So, yes, you should still vaccinate your cat.
To minimize the risk even further, there have been several developments in vaccination. For example, vaccinations are made differently now. Instead of the simple modified live versus killed option, we now have recombinant vaccinations that allow a live non-adjuvanted approach to vaccination against diseases like rabies and feline leukemia virus. These are preferentially used over the adjuvanted killed vaccines that have been heavily implicated in sarcoma formation.
Some vaccines are given in a needle-free manner (such as nasally) to avoid creating a depot of vaccine in the muscle and skin tissues.
Vaccines are divided into core vaccines that all cats should have regardless of their indoor/outdoor lifestyle (rabies and FVRCP distemper vaccines are considered core), while other vaccines are given depending on the cat's realistic risk of exposure.
Vaccines are now given in specific locations so as to control how much inflammation occurs in a given spot.
You can also read a summary of the 2020 vaccination guidelines for cats from the American Association of Feline Practitioners.
Guidelines for Preventing Injection Site Sarcoma
Avoid Unnecessary Vaccination
Be wary of vaccination recommendations that encourage you to vaccinate for every possible disease. Recommendations are highly regional and individualized according to the philosophy of your veterinarian, and they all may have a different philosophy, but the guidelines developed by the American Veterinary Medical Association, and the American Association of Feline Practitioners, are a good place to start (see link above).
Use Live Vaccine when Possible
Live virus vaccines do not employ adjuvant to stimulate the immune system. Because there is a live vaccine involved, a more natural approximation of the infection is achieved, and this stimulates the immune system much better than any adjuvant. The vaccine that has traditionally involved killed viruses (feline leukemia and rabies) can be given in a recombinant form, which means a harmless virus is used to carry the relevant DNA from the target virus through the body. In this way, a live virus is used, but the actual virus of the infection is not, just pieces of its DNA. This sophisticated method is widely used to vaccinate cats against rabies and feline leukemia virus.
Feline Injection Sites
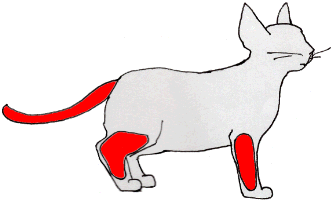
Injections should be given below the elbow/knee or in the tail as depicted. Graphic courtesy of MarVistaVet
Vaccinations Should go in Standardized Areas
Each type of injection and type of vaccine has been assigned an area on the cat's body to be given. This system not only helps researchers track which vaccines are associated with which tumors but also separates administration zones so that inflammation from multiple injections does not add together in one spot. Accepted vaccination guidelines recommend giving vaccines in the areas shown, using the lower limbs or even the tail. These areas have been selected so that, in case a tumor develops, the central body is not involved, and amputating the affected part is possible. This sounds like a radical surgery, and it is; however, fibrosarcoma is a very aggressive and malignant tumor and extreme measures are generally needed to control it. Should a tumor develop, a really wide excision is needed: simply removing the visible "bump" is not going to be helpful in the long term.
The 3-2-1 Rule
Be aware of lumps forming after vaccination (the 3-2-1 Rule). Lumps commonly form in the weeks following vaccination due to the immune stimulation and inflammation centered on this area. These lumps are usually normal and do not represent fibrosarcomas (which generally take years to develop, not weeks). If your cat develops one of these lumps under the skin (they are generally noticed by owners 3-4 weeks after vaccination), the lump may be left alone to resolve naturally. If the lump is still there three months from the time of vaccination, it should be removed and biopsied. Any lumps bigger than 2 cm in diameter (approximately one inch) should be removed no matter how much time has passed since vaccination. Also, any lump should be biopsied if it seems to be getting larger rather than smaller one month after its discovery. (3-2-1 refers to three months post-vaccine, two cm in size, and growing bigger after one month.)
Sometimes one such lump will break open. This event usually means there is an infection rather than that a fibrosarcoma has developed.
Treatment for Vaccine-Associated Fibrosarcomas
Rocky on a Chair

Photo by Dr. Teri Ann Oursler
Injection site sarcomas can be thought of as being similar to an octopus in structure. There is the body that you see, but also far-reaching tentacles that cannot be seen extending far from the visible tumor body. For surgery to be successful, a broad excision is needed, and it is necessary to first determine how far the tumor has spread. Chest radiographs are vital for staging, and CT scanning, if available, is helpful in detecting the extent of the invisible tentacles. If CT scanning is not available, 5 cm (approximately two inches) should be removed around the visible portion of the tumor in all directions, including any bones. Basic blood work, including a feline leukemia virus test, is needed to fully assess the cat for treatment.
If it is possible to remove two inches in all directions around the visible tumor (and consider for a moment how large a volume of tissue this is), the median survival time is two and a half years. The problem is that unless the sarcoma is on a limb that can be amputated, it will not be possible to remove that much of the cat's body. If the complete tumor is not removed, it is almost certainly going to grow back. This situation is where radiation therapy can help a great deal. Whether this should be done before the surgery or after remains controversial and depends on the tumor grade and location. Radiation before surgery can shrink the tumor so as to make surgery more effective. Radiation after surgery can clean up bits of tumor not removed in surgery but must be delayed until the surgery site has healed, and delay can be a problem. Radiation can also be used for palliation, which means the goal is slowing tumor growth rather than curing it; it also means less radiation side effects and expense.
Chemotherapy is sometimes used with radiation and surgery, depending on the grade of the tumor and its location. Your veterinarian may not feel comfortable treating this issue and may refer you to an oncologist to get the most up-to-date treatment.
Our goal here is to create awareness of an emerging problem in veterinary medicine, not to elicit panic. We believe that intelligent decisions about pet ownership require information and education.
What Happens if you Don't do Anything?
Early in the course of this tumor's growth, the tumor is a relatively small yet firm growth on the cat's body, neck or leg. It will probably not be bothering the cat much at this stage, but, as we have discussed, even early in its course this tumor will have far-reaching tentacles whose grasp is deeper and stronger every day. If the tumor is incompletely removed, it is likely to grow back more aggressively. If the tumor is left to progress, it will continue its growth until the skin cannot cover it and it bursts forth. By that time, it will be painful, weepy, stinky, and infected. Surgery will no longer be an option, but it is possible that palliative radiotherapy (radiation) might create some control on a temporary basis. How long does it take to go from a firm lump with good life quality to an infected mass with poor life quality? On average about six months.
Curative treatment is disfiguring and expensive, but currently, it is the only means of addressing this tumor.
Our goal is to create awareness of an emerging problem in veterinary medicine. We believe that intelligent decisions about pet ownership require information and education.