bacterial isolate CDC
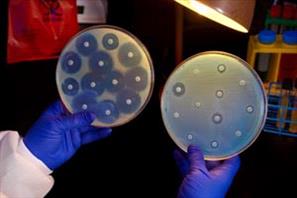
The bacterial isolate on the left plate is susceptible to the antimicrobials in all of the different discs on the plate, which prevents it from growing near the discs. The isolate on the right plate is resistant to all the antimicrobials and can therefore grow near the discs. (Photo by James Gathany of CDC)
The emergence of mcr-1 is a big issue, because if you’re infected by a bacterium that is resistant to most antibiotics, and mcr-1 adds resistance to what might be the drug of last resort, that leaves you with zero treatment options. It’s been stated that mcr-1 heralds the emergence of the first truly pan-resistant bacterial infections – infections that can’t be treated with any antibiotics at all. It’s probably a fair statement.
A report in an upcoming edition of Emerging Infectious Diseases (Zhang et al 2016) describes three people from China infected with mcr-1 harbouring E. coli. One of the individuals worked in a pet shop, so they tested 53 dogs and cats from the store. Pretty concerningly, mcr-1 was found in four dogs and two cats. That’s bad. What makes it worse is that a few different strains of E. coli in these animals carried mcr-1, indicating they had either been infected by multiple (unidentified) sources, or mcr-1 had be passed around between bacteria in the animals’ guts. Four isolates from the dogs and the isolate from the person were the same, supporting transmission between them. Whether that means it went from dog-to-person (along with dog-to-dog) or person-to-dog can’t be discerned. It also cannot be ruled out that the animals and person were infected by some other unidentified source. Either way, this highlights the potential for interspecies transmission of mcr-1 and potentially for the spread of mcr-1 within dog and cat populations, as well as transmission of the gene between bacteria within an individual. None of those are good news, but none are really that surprising.
What is the animal health risk?
Pretty minimal, most likely. Resistance to colistin isn’t too much of a concern since it’s a drug we’re very unlikely to use in animals. Lower profile but more common antibiotic resistant bacteria that we encounter on a regular basis are going to continue to have a greater impact.
What is the public health risk of mcr-1 in companion animals?
That’s a tougher question to answer. It’s probably very low but it’s pretty early to say much with confidence. The odds of any given household pet shedding a bacterium that has mcr-1 are probably very low. Further, if the pet has it, where did it get it? In a lot of situations, it would be from its closest contacts (i.e. people) who probably pose a greater risk of passing it on to other household contacts.
The scenario is probably going to be similar to what we see with MRSA in pets, albeit on a hopefully much smaller scale. MRSA infections in dogs and cats are typically human-associated. They get infected with common human strains and people are probably the ultimate sources of infection. That being said, if an animal is shedding MRSA, it poses some risk of passing it back to the human population. The same would likely apply to some bacteria carrying mcr-1.
What does this mean to veterinarians and animal owners?
It’s just one more reason to use antibiotics right. We need to use them, so we need to make sure that we use them well.
There’s a lot more to the story of mcr-1 and companion animals that needs to be discerned. As the report authors wrote, “companion animals can serve as a reservoir of colistin-resistant E. coli, adding another layer of complexity to the rapidly evolving epidemiology of plasmid-mediated colistin resistance in the community."
Reprinted with permission from Worms and Germs Blog.