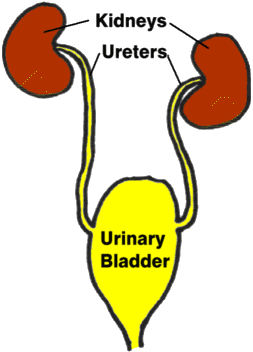
Graphic by MarVistaVet
Note: From a practical standpoint, the terms chronic kidney disease, chronic renal failure, renal insufficiency, chronic kidney failure, and kidney insufficiency all mean the same thing. For simplicity's sake in terms of this article, the term kidney failure will be used to reflect all these terms or conditions.
The kidney is an amazing organ. It is designed to do a lot more than just make urine and get rid of toxins. It also manages hydration, blood pressure, red blood cell production, pH balance in the blood, calcium, and phosphorus balance, and more. Kidneys are made up of millions of filtration units called "nephrons" and we are born with vastly more nephrons than we need to keep healthy. Over time and age, however, nephrons get damaged through the wear and tear of living and they die off. We only need enough nephrons to fill up about 1/3 of one kidney to manage normal kidney function and we start with two full kidneys packed with working nephrons at first but there may come a time when we just don't have enough anymore.
When we don't have enough working kidney tissue to maintain normal function, we are said to have "renal insufficiency," with "renal" being the medical term for the kidney. Kidneys with insufficient function need help to get their work done and a long-term diseased kidney, regardless of its function or lack thereof, has "chronic kidney disease." Chronic kidney disease patients are divided up by what stage of insufficiency they are contending with and what symptoms they have. Treatment is focused on preventing progression of the insufficient function in earlier stages and on maintaining good life quality in later stages.
In the past, we used the term "chronic kidney failure" instead of "renal insufficiency" but this wording sounded far too dramatic and evoked images of ongoing sickness, expensive hospitalization, and doom when management could be as simple as diet change depending on the stage at which the disease is discovered. Early detection is paramount so let us review what the kidneys do and where they might need some help.
What our Kidneys Do/What Insufficient Kidneys Cannot Do
First, it is important to know what normal kidneys do. Kidney function goes far beyond simply making urine. Kidneys are made of millions of processing units called nephrons. These tiny little units are responsible for separating the chemicals you want to keep in your body from the chemicals you need to dispose of. The chemicals to remove are dissolved in water and make up the fluid we all know as urine. So here is what your kidneys do for you and for your pet, what they become unable to do in renal insufficiency, and some of the parameters your veterinarian will want to track.
Water Conservation
Excessive thirst is a warning sign for poor kidney function.

Photo Courtesy of Morguefile.com
Hydration of the body depends not only on water consumed but on water removed. In times of dehydration, the kidney must respond by conserving water. This means that all the materials that the body needs to get rid of still need to be removed, but the kidney needs to do so using the smallest amount of water possible. Similarly, if you drink too much water, the kidney needs to efficiently remove it to prevent dilution of the bloodstream. A pet with insufficient kidney function will not be able to make concentrated urine and will need to drink extra water to process the body's waste chemicals. For this reason, excessive water consumption is an important early warning sign and should always be investigated.
When we analyze a urine sample, one of the most important parameters is the specific gravity. It is a measure of how concentrated a urine sample is. Water has a specific gravity of 1.000. A dilute urine sample has a specific gravity of less than 1.020 (often less than 1.010). A concentrated urine sample would have a specific gravity over 1.030 or 1.040. A failing kidney, by definition, cannot make concentrated urine and the patient must drink excessively to get enough water to get rid of the day’s toxic load.
Toxin Removal
The kidneys remove our metabolic wastes for us. If there is inadequate circulation going through the kidneys or if there are not enough functioning nephrons to handle the waste load, toxins will build up. When the toxins build up and exceed the normal range, a condition called azotemia occurs. If the toxins build up to a level where the patient actually feels sick, they have a condition called uremia. If we can keep our azotemic patients below the uremia level, they will feel pretty normal and have good life quality.
The most important marker of uremia is called creatinine. Creatinine is a by-product of muscle breakdown and is always in small amounts in the bloodstream. The kidney removes it continuously unless there is a kidney function problem. A newer parameter called SDMA (symmetrical dimethylarginine) becomes abnormal much earlier than creatinine does and is becoming more commonly tracked. We are able to stage a patient's kidney disease based on creatinine blood level and SDMA level (see the staging section below). Another marker is the BUN, which stands for blood urea nitrogen. This parameter is similar to creatinine but is influenced by dietary protein as well as kidney function. These three markers are central to determining the severity of a kidney problem.
Calcium/Phosphorus Balance
The balance between calcium and phosphorus in the blood is really important. Too much of one or the other will lead to crystals forming in body tissues and bones to the extent that they may actually become rubbery. The kidney plays an important role in this balance and when kidney function is lost, phosphorus levels begin to rise. Therapy for insufficient kidney function requires monitoring phosphorus levels and the use of diet and medications to keep phosphorus levels in a reasonable range.
Sodium/Potassium Balance
The kidney plays a major role in controlling electrolyte balance as well. In particular, conserving potassium is an important aspect. Insufficient kidneys lose their ability to conserve potassium and potassium levels begin to drop, leading to weakness. Potassium supplements are commonly needed in the treatment of kidney failure.
Blood Pressure Regulation
Blood pressure sensors in the kidney help regulate blood pressure in the body. When these are damaged, hypertension (high blood pressure) can result and can damage the kidney even more. Blood pressure is commonly measured in kidney failure patients.
Protein Conservation
There are a lot of important proteins circulating in the bloodstream and it is crucial that they are not lost in the urine. The nephron possesses a filtration system that keeps the protein in while removing harmful wastes. If this filtration system is damaged (glomerular disease) then a much more severe form of kidney failure results. Screening for this damage is an important aspect of staging kidney failure and a test called a urine protein: creatinine ratio is often included in the testing profile to assess this condition.
Red Blood Cell Production
The kidney produces a hormone called erythropoietin. This hormone tells the bone marrow to make more red blood cells. In the absence of this hormone, non-responsive anemia occurs and can get so bad that a transfusion is necessary. Erythropoietin can be given by injection to treat this problem but there are some potential pitfalls in doing this as will be discussed in a later article. Hematocrit and packed cell volume (PCV) are measures of red blood cell volume commonly monitored in kidney patients.
pH Balance
Metabolic processes require a narrow pH range for efficiency. The kidney also regulates this balance and if it cannot, intervention, usually in the form of fluid therapy, is necessary.
That's a lot of tasks for a pair of kidneys to handle! With chronic kidney disease/renal insufficiency, chances are at least one of these tasks is not moving along smoothly. There may or may not be any symptoms when the disease is discovered but the goal is to slow the progression to the point where symptoms develop. If there already are symptoms, the goal becomes controlling the symptoms and maintaining good life quality.
Once kidney disease has been discovered, the next step is staging and evaluating any other aspects of the above function list that may not have been covered. Typically animals need special food and possibly medications depending on symptoms. Very advanced cases will likely need hospitalization, intravenous fluids, and possibly assisted feeding to get to where they can resume a more normal life at home. As mentioned, early screening is especially important as it is much easier to slow the progression of disease than it is to reverse it.
STAGING KIDNEY DISEASE
Kidney disease is either discovered via wellness screening tests of apparently healthy animals or during the course of the evaluation of patient illness. As mentioned, what we do for the patient will depend on the stage of the disease. The International Renal Interest Society (IRIS) has determined a staging system based on the creatinine level and SDMA level found on a blood test (see Toxin Removal section above). Patients in Stage 1 or 2 rarely have any symptoms related to their disease and those in Stage 3 or 4 usually have symptoms to control.
The chart below stages dogs and cats according to their Creatinine and SDMA levels. Once the patient has been staged then further testing for "sub-staging" begins.
Table 1: Creatinine Values for Each IRIS Stage listed in US, International, and SDMA Units
| |
Units
|
Stage I
(pre-failure)
|
Stage II
(mild failure)
|
Stage III
(moderate failure)
|
Stage IV
(severe failure)
|
|
Dog
|
mg/dl
μmol/l
SDMA μg/dl
|
<1.4
<125
<18 mcg/dl
|
<1.4-2.8
<125-250
<18-35 mcg/dl
|
<2.9-5.0
<251-440
<36-54 mcg/dl
|
>5.0
>440
>54 mcg/dl
|
|
Cat
|
mg/dl
μmol/l
SDMA μg/dl
|
<1.6
<140
<18 mcg/dl
|
<1.6-2.8
<140-250
<18-25 mcg/dl
|
<2.9-5.0
<251-440
<26-38 mcg/dl
|
>5.0
>440
>38 mcg/dl
|
Sub-staging of kidney disease involves screening for urine protein loss and measuring blood pressure. A urine protein: creatinine ratio is performed on a urine sample and the protein amount is classified as either non-proteinuric, borderline proteinuric, or proteinuric. Blood pressure is checked and the patient is classified as normotensive (normal), borderline hypertensive, hypertensive, or severely hypertensive. The ultimate classification for the patient will reflect all of these things ("Stage 3, non-proteinuria, normotensive" would be an example). Further testing and monitoring are determined based on what the actual parameters are. For more details on these substages, see the articles on glomerular disease, and hypertension.
Stage I is mostly for pets that are known to have kidney disease based on abnormal ultrasound or their slightly elevated SDMA. We check their blood pressure and urinary protein levels, and screen for urinary tract infections. If abnormalities are found, they are usually checked quarterly for any sign of progression.
Stage 2 is where diet change to a renal diet is typically recommended with the idea being that the earlier this is started, the more likely the pet will accept it. The same type of screening is performed as with Stage I, only now we need to start watching the phosphorus levels so they don't rise above 4.6 mg/dl. Also, potassium levels may begin to drop especially in cats. Both of these factors are helped by using a renal supportive diet but if that proves inadequate, medications may become needed.
In Stage 3, the patient is likely to be showing some symptoms such as reduced appetite or occasional nausea. In addition to the tests of Stages I and 2, it is in Stage 3 that we start paying attention to red blood cell numbers and blood pH. This is a good time to consider the use of calcitriol (active vitamin D supplementation) if one is going to do so.
In Stage 4, the patient is almost certainly showing symptoms and it becomes important to be sure the patient is eating enough calories to maintain a healthy weight. Similar concerns exist as for the first three stages but a phosphorus level of 4.6 mg/dl is probably unrealistic at this point and a better goal is 6.0 mg/dl. Fluid support at home is a good idea. This may mean adding water to the food, giving fluids under the skin (subcutaneous fluids), or even a stint of hospitalization and IV fluids to drive the numbers down.
Many patients are not diagnosed with kidney disease until they are far past a creatinine of 5.0 mg/dl. It is not unusual for sick patients to come to the vet and have creatinine values of 10 mg/dl or higher. At this point, more aggressive treatment will be needed to stabilize the patient and the goal is going to be improving the dysfunction to a level where the patient has acceptable life quality and comfort at home. Transitioning to a new lifestyle will take some time. (For example, appetite and comfort must be restored but changing to a renal support diet may be something for further down the treatment path when more stability has been achieved).
A Note on Pyelonephritis
Pyelonephritis is another name for kidney inflammation and usually means kidney infection. Patients get kidney infections when a bladder infection goes unnoticed or incompletely treated long enough and the bacteria go up the ureters into the kidney where they set up shop and cause damage and pain. This form of kidney failure has the most potential to reverse or partially reverse, so it is important to culture the urine for it early. Urinalysis is frequently unable to detect infection in this situation as the patient drinks so much water that the visible markers of infection are diluted out and cannot be found. The infection also will produce a significant amount of urinary protein so the patient will be sub-staged incorrectly if an infection is not ruled out.
A Special Note on Ureteral Stones
The ureter is the tube that connects the kidney to the bladder and urine should constantly be flowing through it. Often in age (plus with calcium/phosphorus imbalance), mineralization will occur in the kidney. This may or may not be a problem depending on how big and how plentiful the mineral deposits are but sometimes a mineral deposit will break off and get lodged in a ureter. This can obstruct the ureter completely and the backlog can destroy the kidney. Or it can partially obstruct the ureter, causing obstruction and then the relief of obstruction as it rolls down the ureter and (hopefully) into the bladder where it will not cause trouble. A spike in creatinine can be a clue that this has happened and if one acts quickly intervention may be possible. For this reason, some kind of imaging of the kidneys is recommended early in the course of kidney disease and periodically after.
The bottom line is that there is a wide range of treatments when a patient has insufficient kidney function and a lot of monitoring is needed to keep on top of all the aspects. Each patient will have a different stage and a different constellation of issues to contend with. Some will need only a diet change, and some will need ongoing fluid therapy at home or hospitalization. The prognosis depends on all the factors involved. Your veterinarian will let you know what your particular pet needs and will be watching many different lab tests to keep control of your pet's condition.
In Summary:
- From a practical standpoint, the terms chronic kidney disease, chronic renal failure, renal insufficiency, chronic kidney failure, and kidney insufficiency all mean the same thing.
- The kidney’s job is more than just to make urine and get rid of toxins. Additionally, the kidney manages hydration, blood pressure, red blood cell production, pH balance in the blood, calcium and phosphorus balance, and more.
- Over time, kidney cells can become damaged. When there is not enough working kidney tissue to maintain normal function, it is called “renal failure”. A long-term diseased kidney, regardless of its function or lack thereof, has "chronic kidney disease."
- Hydration of the body depends not only on water consumed but on water removed. In times of dehydration, to keep this balance, the kidney will remove the toxins using the smallest amount of water needed.
- If over-hydrated, the kidney must remove excess water to prevent dilution of the bloodstream.
- A failing kidney cannot make concentrated urine, and the patient must drink excessively to get enough water to get rid of the day’s toxic load. Excess water consumption by your pet could be an early warning sign of kidney disease.
- If there is inadequate circulation going through the kidneys or if there are not enough functioning kidney cells to handle the waste load, toxins will build up.
- If concerned about possible kidney disease and toxin levels, your veterinarian will order a urinalysis and blood work for your pet. Markers in the urine and blood will show the presence and severity of a kidney problem.
- Levels of kidney disease are labeled by “stages,” i.e., I (pre-failure), II (mild failure), III (moderate failure), IV. (severe failure). How far the disease has progressed will determine treatment.
- Treatments can be combinations of fluid therapy, diet changes, medications, and possibly vitamin supplementation. On-going examinations and laboratory tests will be a part of the treatment as your pet is monitored for changes to their condition.
- Prognosis depends on the stage of the disease and factors involved. Back to top
©2024 Veterinary Information Network®, Inc.