
Hackett ventilator 288

Screenshot from Facebook video
Dr. Tim Hackett loaded a Siemens Maquet Servo-i ventilator into his truck on Friday. The Colorado State University Veterinary Teaching Hospital is providing this ventilator and others, normally used for animal patients, to area hospitals for human patients experiencing respiratory failure due to COVID-19.
Dr. Tim Hackett rolled a life-support ventilator up to the automatic doors of UC Health Poudre Valley Hospital into the waiting hands of masked and gloved health care practitioners on Friday. The James L. Voss Veterinary Teaching Hospital at Colorado State University in Fort Collins had purchased the ventilator for the care of critically ill dogs, cats, rabbits and other animals. Now it, along with other veterinary ventilators belonging to CSU, will be used to help COVID-19 patients with respiratory failure.
A veterinarian, Hackett is the director of the teaching hospital and a professor of emergency medicine at CSU. "It will be such a boost to everyone around here to know that something that we had will be used to meet the needs of our neighboring health care system," he told the VIN News Service.
The novel coronavirus that causes COVID-19 attacks the lungs and can lead to pneumonia and acute respiratory distress syndrome. Ventilators deliver air to the lungs through a tube placed in the windpipe and do the work of breathing for patients who can't breathe on their own. For some COVID-19 patients, going without a ventilator means certain death.
There aren't enough ventilators to meet demand, and no easy way to manufacture more quickly, according to reports in The New York Times and elsewhere.
Aware that veterinary ventilators are the same as those used in human medicine, critical care specialists at veterinary schools and specialty emergency hospitals realized they could help narrow the gap.
On their own and in concert with one another during the past couple of weeks, they began taking stock of their resources and reaching out to medical hospitals to see how they might help.
Dr. Beth Davidow, president-elect of the American College of Veterinary Emergency and Critical Care (ACVECC), spearheaded an effort to create a nationwide inventory of ventilators available for human medical facilities. Davidow is a critical care veterinarian in the Seattle area, where the first case of COVID-19 in the U.S. was reported in January. More than 367,000 people have been infected worldwide and more than 16,000 have died due to the disease, as of this morning.
Davidow ventilator 288
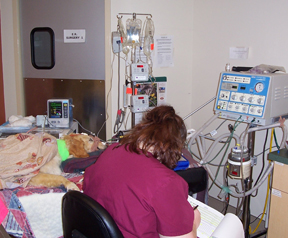
Dr. Beth Davidow photo
A veterinary assistant monitors a golden retriever on a life-support ventilator. The 7-year-old dog had had a seizure in 2007 while running on a beach in the Seattle area, collapsed and nearly drowned. In acute respiratory distress, she was put on life-support for several days, and eventually made a full recovery. Ventilators used by veterinarians, like this one, are being shared with human hospitals in response to the COVID-19 crisis.
"I think people on the human side forget we're a resource," Davidow said about veterinary medicine. "Realizing we're there might be worth thinking about."
As of Saturday, 160 veterinary facilities had added ventilators to ACVECC's spreadsheet. The list is not public because it contains personal cell phone numbers of veterinary critical care specialists so that physicians can reach them directly in an emergency. The information is available to practitioners through the Society for Critical Care Medicine, the American Medical Association and the American Veterinary Medical Association, according to Davidow.
Veterinary hospitals with life-support ventilators to donate can submit their information via this form.
Donating a ventilator is not an easy decision for veterinarians. It may mean that, down the road, there is no ventilator for a very sick animal that needs it.
"These unprecedented times require unprecedented sacrifices," ACVECC president Dr. Ken Drobatz said on Friday. Drobatz is the director of Emergency Services at Ryan Hospital at the School of Veterinary Medicine of the University of Pennsylvania. He said his team sent two ventilators to Penn Medicine, the university's human health system.
Ventilators vary
While using a ventilator last used by an Irish wolfhound may disconcert some non-veterinarians, Davidow says it doesn't make a difference.
"The ventilator delivers the air," she explained. "It is the driving force. What is important is the tubing, and the tubing is sterilized between patients."
The vast majority of "veterinary" ventilators are made for humans and used for animals, or are refurbished human ventilators marketed to the veterinary profession.
The more important distinction in terms of the coronavirus pandemic is the type of ventilator. Broadly, there are two types: life-support ventilators and anesthetic ventilators. Anesthetic ventilators are intended to use for short periods while a patient is under anesthesia. In general, anesthetic ventilators provide 100% oxygen flow.
Giving 100% oxygen for too long can lead to oxygen toxicity and injure the lungs. Air is comprised of about 21% oxygen.
Life-support ventilators are designed for the longer haul. They can be adjusted to vary the amount of oxygen, pressure and volume delivered to the patient's lungs.
The inventory at CSU's veterinary hospital until Friday was three life-support ventilators and 30 anesthetic ventilators. All could be made available as needed. The one delivered to Poudre Valley Hospital and another bound for a hospital in Greeley, Colorado, where patients needing ventilators outnumber machines, are both life-support ventilators. Whether anesthetic ventilators can be useful to support patients with COVID-19 is up for debate.
Using anesthetic ventilators in these circumstances requires a certain level of expertise, Hackett said, and "could be effective with a trained person operating them." A "limiting factor" could be having enough trained personnel to operate them, he said.
The price on ventilators varies greatly, from $5,000 to $7,000 for an older, refurbished basic model, to six figures for newer models, according to Davidow.
How to help
Drives for donations of supplies — from personal protective equipment, known as PPE, to medical machinery such as ventilators — are becoming a common feature of life during the coronavirus pandemic.
The solicitations cause some to be leery. For example, Dr. Danielle Huff, a veterinarian in Redmond, Oregon, was suspicious when her hospital received an email seeking information about ventilators and monitors "that might be able to supplement support for patients impacted by the pandemic." The email came from a personal email account, professed to be from an organization Huff knew hadn't endorsed the request, and contained terminology that raised "red flags" for her.
Always wary about potential scam emails, Huff said she is especially on alert during this crisis.
"We're such kind-hearted professionals, we want to help at all costs ... We should not lose our equipment while trying to help others."
While caution is advisable, in this case, VIN News contacted the sender and determined that the email was part of a sincere, independent effort to help hospitals facing shortages during the crisis.
The AVMA is working with national organizations such as the American Association of Veterinary State Boards and the Association of American Veterinary Medical Colleges to provide guidance and opportunities for veterinarians wanting to help, according to an update sent to members on March 19.
ACVECC's Drobatz recommended veterinarians speak directly with hospitals before committing to send valuable equipment.
Meanwhile at CSU, Hackett has ideas that go beyond ventilators. He has provided information to Colorado emergency planners about an empty research building at the veterinary school that could be converted into a hospital. He also imagines a time when veterinarians themselves could be called upon.
If that time comes, he said, "We all feel like we could be a competent set of hands to assist medical teams."