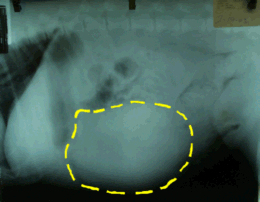
This radiograph of a dog's abdomen shows a dramatically enlarged spleen. The spleen is outlined. Photo by MarVistaVet
Hemangiosarcoma is a malignant tumor of blood vessel cells. With the exception of the skin form - which can often be eliminated by surgery - a diagnosis of hemangiosarcoma is bad news. This tumor is associated with serious internal bleeding and rapid internal spread. Fortunately, it is not a completely without therapy options and, as long as expectations are realistic, temporary remissions are possible.
When found internally, this tumor is associated with serious internal bleeding and rapid internal spread. Treatment options and prognosis depend on the location involved. Hemangiosarcoma is a common tumor in dogs but we have included feline information at the end of this article.
Hemangiosarcoma in Dogs
Hemangiosarcoma can theoretically arise from any tissue where there are blood vessels (which amounts to anywhere in the body) but there are three classical locations that account for most cases:
- Skin and subcutaneous forms
- Splenic forms
- Heart-based forms
The Skin Forms
The skin forms of hemangiosarcoma are the best types to have as they are the most easily removed surgically and thus have the greatest potential for complete cure.
The skin forms of hemangiosarcoma are classified as either dermal and subcutaneous (also called hypodermal). The true skin form looks like a rosy red or even black growth on the skin. This form is frequently associated with sun exposure and thus tends to form on non-haired or sparsely haired skin, such as on the abdomen, or on areas with white fur. Dogs with short white-haired fur (such as Dalmatians and pit bull terriers) are predisposed to developing this tumor. Approximately one-third of cases will spread internally in a malignant way if given enough time, so it is important to remove such growths promptly.
The biggest problem with the dermal hemangiosarcoma is that it frequently arises in multiple spots within a broader expense of skin. Isolated growths can be easily removed but when a large area of skin is involved, surgical removal becomes trickier and often multiple surgeries are needed to remove multiple small tumors.
The dermal hemangiosarcoma has a fair prognosis as long as it is removed before it can invade to the subcutaneous tissues.
Subcutaneous or Hypodermal Hemangiosarcoma
Hemangiosarcomas that develop in the subcutaneous tissue (not on the skin but under it) or spread to the subcutaneous area from the outer skin behave more malignantly. The overlying skin is often totally normal on top of a subcutaneous hemangiosarcoma and often the surgeon is surprised to find a dark blood-red growth under the skin when the tumor is removed. A subcutaneous hemangiosarcoma should be treated as cancer and an oncologist should be consulted for therapy beyond surgical removal.
- Since up to 60 percent of hypodermal hemangiosarcomas spread internally, staging becomes important after this tumor is identified (see below).
- Surgery alone has been associated with a 172-day (approximately 6 month) median survival time.
What to Know When a Skin Growth Biopsy Comes Back as Hemangiosarcoma
The biopsy report will indicate whether or not all of the growth was removed. If the tissue completely surrounding the growth is normal, this indicates that the growth has been removed completely and that it should not grow back.
Because the subcutaneous form of hemangiosarcoma wants to spread, staging is a good idea to determine the extent of the disease. Knowing how far the tumor has spread will establish appropriate treatment options and provide information on life-expectancy.
- Chest radiographs: hemangiosarcoma tends to spread to the lungs. Advanced tumor spread can be found with this simple test. (Spots of tumor spread must be 3 mm in diameter to be large enough to be visible on a radiograph.)
- Ultrasound of the belly: specifically the spleen. Even a small splenic hemangiosarcoma should be detectable with ultrasound.
- Ultrasound of the heart: even a small heart-based hemangiosarcoma should be detectable with ultrasound.
After staging, consultation with an oncology specialist is likely to provide the most up-to-date recommendations.
Hemangiosarcoma of the Spleen
The spleen is a fairly deep-seated abdominal organ that tends to go unnoticed unless it grows unusually large. Splenic growths have the unfortunate tendency to break open and bleed profusely regardless of whether they are benign or malignant. While a splenectomy (removal of the spleen) certainly ends the prospect of this type of life-threatening sudden bleed, splenic hemangiosarcoma is still a rapidly spreading malignancy.
When a splenic mass is detected, it may not be possible to tell before a splenectomy whether or not the mass is malignant (though certainly basic testing is done in an attempt to determine this). Chest radiographs are generally performed pre-operatively to check for evidence of cancer spread as well as for evidence of a concurrent heart-based tumor (heart-based hemangiosarcoma and splenic hemangiosarcoma occur together in 8 percent of splenic hemangiosarcoma patients). If possible, abdominal ultrasound can be done to look for tumor spread to other organs prior to surgical exploration. If tumor spread is evident, it may not be worth continuing on to surgery and certainly if tumor spread is not evident, that does not mean that the tumor is benign. The spleen will need to be removed and sent to the lab for analysis in order to determine if it is benign or malignant.
- Median survival with surgery only (i.e. no chemotherapy) is 19 to 86 days for hemangiosarcoma. Benign hemangioma, however, is cured with surgical removal. It may not be possible to tell benign hemangioma from malignant hemangiosarcoma without removing the spleen and sending it to the lab.
- Chemotherapy extends survival to approximately 3-6 months on the average, assuming there is no evidence of tumor spread at the start. Metronomic chemotherapy protocols (smaller doses and fewer side effects) show similar survival statistics compared with more conventional chemotherapy protocols.
- About 40 percent of bleeding splenic tumors are benign hemangioma and 60 percent are malignant hemangiosarcomas.
- Many patients are bleeding internally at the time of diagnosis and require emergency surgery.
- Because there is so much potential to bleed during surgery, even the patients who are not actively bleeding may need a blood transfusion before surgery.
Obviously, this is a highly malignant tumor with limited treatment options. Often a pet owner has never heard of this tumor until a beloved pet is suddenly in the middle of an internal bleeding crisis and decisions must be made quickly. Clearly, the best outcome results when the tumor turns out to be benign but, as mentioned, it may take a risky and expensive surgery to determine this.
Any breed of dog can be affected but a predisposition has been identified in the German shepherd dog, the golden retriever, and the Labrador retriever. Median age at the time of diagnosis is 10 years.
Yunnan Baiyo: A Chinese Herbal
It is worth mentioning this product as it may be the only option for a dog that is not going to have surgery. A splenic tumor will periodically bleed and clot again and again until the point comes when the bleed is simply too big and the patient succumbs to the blood loss. This herb has been found to improve clotting tendencies and may give the patient an edge against the tumor. Ask your veterinarian for instructions on how to use this product. It comes as either a powder or in capsules.
A bleeding episode will manifest as weakness, chill and pale gums. A snug bandage wrap around the belly may stop the bleeding in the home setting. Obviously, this kind of first aid approach is not a replacement for emergency medical treatment but if you are doing home hospice care, it may be appropriate.
Heart-Based Hemangiosarcoma
Like the splenic hemangiosarcoma, the heart-based hemangiosarcoma exerts its life-threatening effects by bleeding. Tumors are generally located around the right side of the heart base.
The heart is enclosed in a sac called the pericardium. When the hemangiosarcoma bleeds, the blood fills up the pericardium until it is so full that the heart inside is under so much pressure that it has no room to fill with the blood it needs to pump.
In chest radiographs, the heart looks globoid (spherical). In fact, the heart is of normal shape but all that can be seen is the large, round heart shadow of the pericardium filled to capacity with blood. Ultrasound is needed to truly see the effusion.
This condition, if allowed to progress, results in an emergency circulating collapse called a pericardial tamponade and can only be relieved by tapping the pericardium with a needle and withdrawing the excess fluid.
- 63 percent of heart-based hemangiosarcomas have evidence of tumor spread at the time they are discovered.
- Survival time for surgery alone (removing the pericardium and snipping off the heart-based hemangiosarcoma) is approximately 1 to 3 months. In a study published in the Journal of the American Veterinary Medical Association in February 2005, 23 dogs with this type of tumor were studied. Of the dogs that had surgery, approximately half of them had some sort of post-operative complication, though most complications were minor; and 87 percent survived and were released to go home from the hospital. Median survival time for dogs that had surgery without chemotherapy was 43 to 118 days (depending if the tumor was in the right atrium or just in the auricle, which is the small ear-like area adjacent to the atrium).
- Eight of the dogs that survived surgery went on to receive chemotherapy and these individuals had much longer survival times (median survival of 175 days vs. 42 days for dogs who had surgery without chemotherapy).
Chemotherapy is necessary to create a substantial improvement in survival time. The most current protocol involves injectable Adriamycin (doxorubicin) every three weeks and oral cyclophosphamide at home for three days out of the week.
On the Horizon
Immunotherapy is an active area of research with the idea being to find a vaccine that will induce the patient's own immune system to seek and attack the tumor. This area appears promising but is still in an experimental stage. Antiangiogenic therapy involves reducing the tumor's ability to generate blood vessels to feed itself. This area is also investigational at this time. It may be possible for your pet to participate in a funded study.
Hemangiosarcoma in Cats

Photo by Dr. Teri Ann Oursler
As cancers go in cats, hemangiosarcoma is not a common one as it is for dogs but cats still can get one. There appear to be four main types of hemangiosarcoma in cats:
- Dermal (in the skin)
- Subcutaneous (under the skin)
- Visceral (involving internal organs)
- Oral (usually growing from the gums)
Recent studies indicate that the dermal and subcutaneous forms are the most common. These forms tend to develop on the head, which suggests that sun exposure is a risk factor. For the dermal and subcutaneous forms of feline hemangiosarcoma, surgical removal is the chief treatment and is the most likely to be curative for dermal forms. Subcutaneous hemangiosarcomas are more difficult to remove completely and have a 60 percent recurrence rate after surgery. The visceral form is the most aggressive form with approximately 30 percent of cats being far gone enough to warrant euthanasia at the time of initial diagnosis (or having already died with the diagnosis being made on a post-mortem exam).
In dogs, adding chemotherapy to surgery has been helpful in extending the disease-free interval. Certainly protocols are available for cats, but so few cats have been treated that statistics comparing protocols or even comparing surgery plus chemotherapy treatment vs. surgery alone are not available.
One useful finding that has emerged from retrospective studies is the significance of the mitotic figure count on the biopsy sample. A mitotic figure is a cell that is in the process of cell division when it is fixed in formaldehyde. Since rapid cell division is a feature of malignancy, the number of mitotic figures seen on a slice of tissue can indicate how aggressive a tumor is. Apparently more than three mitotic figures per high power microscope field indicates a much shorter survival time than would be achieved in a case with a smaller number of mitotic figures. The mitotic figure count is reported by the pathologist when the biopsy sample is read, although it may have to be specifically requested.