Neurotransmitters
In general, psychotropic medications affect a relatively small group of neurotransmitters. Knowing the major functions and effects of inhibition and enhancement of transmission of these neurotransmitters is extremely helpful when prescribing medications.
Amino Acids
The amino acids are the workhorses of the brain neurotransmitters. Gamma-aminobutyric acid (GABA) is the most widespread inhibitory neurotransmitter in the brain. GABA is involved in the inhibition of vigilance, anxiety, muscle tension and memory enhancement. Glutamate works in an excitatory capacity in the brain. It is the major mediator of excitatory signals in most aspects of normal brain functioning including cognition, memory and learning. The most commonly used veterinary medication classes which affects GABA are the benzodiazepines and anticonvulsant classes. Natural compounds which affect GABA are: alpha casozepine, Magnolia officinalis, Phellodendron amurense, Souroubea, Plantanus and l-theanine. L-theanine and magnolia-phellodendron combinations also act as glutamate antagonists. The products which contain these compounds are discussed in Making Medication Choices.
Gabapentin is an anticonvulsant, antineuralgic used for chronic pain and anxiety. It can be used as a sedative for disorders which interrupt sleep or as a previsit pharmaceutical. It has its effect by closing presynaptic calcium channels thereby diminishing neuronal activity. It doesn’t have any action directly on GABA.
Monoamines
The monoamines include, but are not limited to norepinephrine, serotonin, and dopamine. These three neurotransmitters are concentrated in the hypothalamus, limbic system and other midbrain areas. There is a significant amount of overlap in the effects of these neurotransmitters on the behavior of animals. See Image 1 below.
| Image 1 | 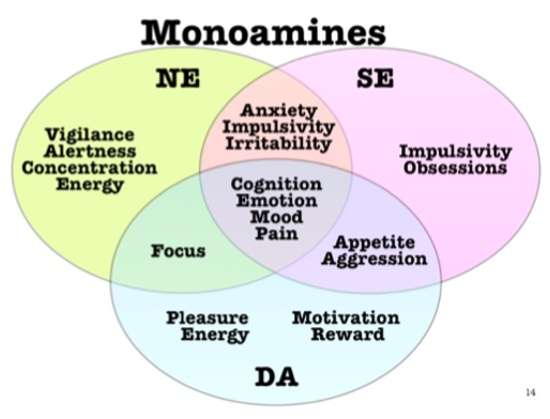
|
|
| |
In addition, the inhibition or enhanced release of one in many cases affects the release or inhibition of another. For example, a medication which only directly affects serotonin, can indirectly through the mechanism of inhibition or enhanced release of serotonin affect norepinephrine.
The monoamines can further be divided up into catecholamines and indoleamines. The catecholamines of interest are norepinephrine and dopamine. Norepinephrine affects alertness, concentration, energy levels, anxiety, impulsivity and irritability as well as attention span. Dopamine in addition to affecting attention span, affects pleasure, reward, motivation, and drive.
Serotonin is an indoleamine. Similarly to norepinephrine, it affects anxiety, impulsivity, and irritability. In addition, if affects obsessive thoughts, compulsions and memory. Norepinephrine, dopamine, and serotonin are all involved in mood stabilization and cognitive function.
Knowing which medications affect which neurotransmitters can guide the practitioner as to how to make medication choices. It can also immediately give the veterinarian and idea of the potential side effects and interactions of that particular medication. See Image 2 and 3 below.
| Image 2 | 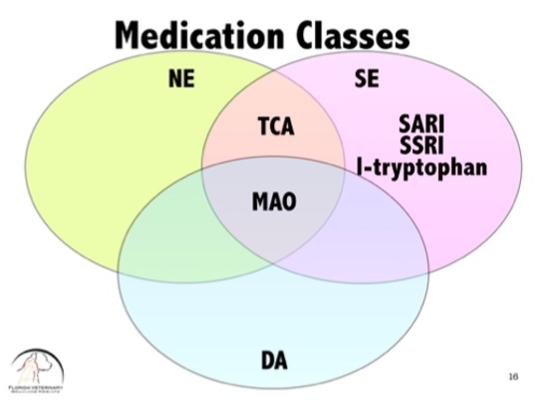
|
|
| |
| Image 3 | 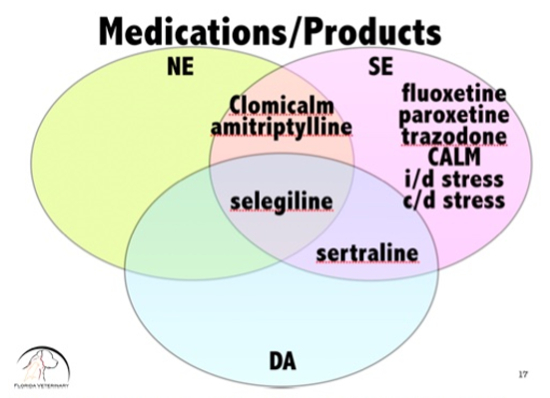
|
|
| |
The monoamines are generally stored in vesicles until they are ready to be released into the nerve synapse. When they are released, they may bind with receptors on post-synaptic neurons as would be expected causing an action potential in that neuron. After binding, the neurotransmitter is released from the receptor into the synapse. Two enzymes are responsible for the breakdown of monamines: monoamine oxidase (MAO) which breaks down serotonin, dopamine and norepinephrine and catechol-o-methyl transferase which breaks down norepinephrine and dopamine. These enzymes are present in the nerve synapse and inside of the neuron. After release from binding into the nerve synapse, the monoamine neurotransmitter is taken up into the nerve and re-manufactured to be stored in vesicles within the neuron ready to be released again.
Generally, antidepressants which are the most commonly used medication for the treatment of emotional disorders in animals involving impulsivity, aggression, anxiety and fear have their effect by blocking the reuptake of the neurotransmitter into the cell thus increasing the ratio of neurotransmitter to receptor or blocking the dissolution of the nerve transmitter itself by blocking the effect of the particular enzyme that breaks it down.
The most well accepted theory as to why antidepressants are effective involves the depletion of neurotransmitters in the brain of affected animals. An aggressive animal is presumed to have a depletion of serotonin, for example. The depletion of serotonin causes an upregulation of the postsynaptic neurotransmitter receptors. Think of this as an increase in the number of receptors available for binding. Administration of selective serotonin reuptake inhibitors (SSRIs) such as fluoxetine and sertraline, cause an increase in the amount of serotonin available for binding increasing the ratio of serotonin to receptors in the nerve synapse. This causes the down regulation of the receptors on the post-synaptic neuron increasing the ratio of serotonin to receptors.
Serotonin reuptake inhibitor/antagonists (SARI) inhibit the serotonin reuptake transporter and antagonize the serotonin 2A receptor on the postsynaptic neuron. SARIs, such as trazodone, block the serotonin reuptake inhibitor at the presynaptic neuron to a lesser extent than the SSRIs, however, they have a powerful action in the blockade of the serotonin 2A receptor. The blockade of the serotonin 2A receptor indirectly increases the stimulation of the presynaptic neuronal autoreceptor.
Monoamine oxidase inhibitors such as selegiline (Anipryl®) function by blocking the breakdown of dopamine by inhibition of MAO. Tricyclic antidepressants such as clomipramine (Clomicalm®) and amitriptyline (Elavil®) inhibit the reuptake of norepinephrine and serotonin. In addition, they cause a blockade of muscarinic cholinergic receptors, H1 histamine receptors and alpha1 adrenergic receptors. The multi-action of this class of medications causes many clinicians to avoid using them in older patients. Patients may experience dry mouth, and sedation among other side effects.
There are at least five benzodiazepine receptor subtypes. Different receptor subtypes are found in different areas of the body. For example, the benzodiazepine 1 receptor is found primarily in the cerebellum. The GABA A receptor is allosterically modulated by multiple other receptors including the benzodiazepine receptor site. So, benzodiazepines have their effect primarily on GABA. When GABA and a benzodiazepine bind together at the GABA A receptor, the effect is greatly amplified. When a benzodiazepine binds by itself, there is no effect on the GABA A receptor. When GABA binds by itself to its own receptor, the effect is substantially less than when a benzodiazepine is also bound to the benzodiazepine receptor site on the GABA receptor. Like many team efforts, the final outcome is much greater than the sum of its parts.
Acepromazine is a phenothiazine neuroleptic agent and a postsynaptic dopamine antagonist. Through it’s action on dopamine 2 receptors, it causes sedation. In veterinary medicine, it is used as a sedative. It is not used as an anxiolytic.
Clonidine is a centrally acting alpha 2 agonist affecting alpha 2, A, B and C receptors. It reduces in SNS arousal and nociceptive pain at lower dosages; and causes sedation at higher dosages. It can be used as a pre-visit pharmaceutical or a short term arousal reliever.3
Often, attempting to understand how a medication works can seem tedious. However, once you understand how a given medication affects the body, how it affects other neurotransmitters indirectly, or the requirement of one neurotransmitter for the other to cause an effect, it makes the selection of medications much more efficient and effective.