L. Findji
Having to close a large or challenging wound is common in small animal surgery, whether it be after tumour resection or in traumatised patients. Simple primary closure, combined when needed with tensionrelieving techniques, allows closure of most wounds in small animals, thanks to the laxity of their skin. Frequently, however, the skin surrounding the wound edges needs to be undermined to free the loose skin around the wound and allow such simple primary closure. Whenever simple primary closure is not possible, reconstructive techniques should be considered. As a rule, the safest, simplest and cheapest option should be preferred, equating to choosing the lowest available technique on the "ladder" of reconstruction techniques. The 5 steps of this ladder, from the lowest to the highest are simple closure, local flaps, axial pattern flaps, distant flaps/free grafts, and microvascular flaps/other advanced techniques. This first part will focus on vascular anatomy and local flaps.
Vascular Anatomy of the Skin
Understanding the organisation of the cutaneous vasculature is critical for skin reconstruction.
In dogs and cats, the skin is vascularised by 3 plexi: the subpapillary, cutaneous and subdermal plexuses. The two most superficial plexuses depend on the subdermal plexus, which is therefore the most important to preserve. This subdermal plexus lies in depth of the hypodermis. In regions of the body where a panniculus muscle is present (trunk, neck), the subdermal plexus runs immediately deeply and superficially to it. As a practical consequence, when the skin is undermined for primary closure or performance of a skin flap, it must be elevated in depth of the panniculus muscle. In areas where no such muscle is present, the skin must be elevated as close as possible from the underlying fascial or muscular plane.
Local Flaps
Skin flaps are either subdermal (relying on the subdermal vascular plexus) or axial (relying on a direct cutaneous artery). Subdermal flaps are subdivided in local and distant flaps.
Subdermal flaps are sometimes referred to as "random" flaps, as they rely on the random subdermal plexus to vascularise the elevated skin. This means that these flaps can be harvested in any location and direction. However, the perfusion pressure of the elevated skin has to be estimated as an empirical statistical notion, as the potential presence and direction of direct cutaneous arteries supplying the elevated skin are unknown (Figure 1a). As a consequence, these flaps can only be elevated on a limited length, and their base needs to be at least as wide as their free end. As an empirical rule, subdermal flaps should only be 1.5 to 2 times longer than they are wide.
Local flaps include advancement (Figure 1b), rotation (Figure 1c), transposition (Figure 1d) and interpolation flaps, depending on the way the excess (loose) skin is transferred to the wound. These flaps are elevated from skin adjacent to the wound. The interpolation flaps involve a staged reconstruction on the same principle as that of distant flaps (see later). It is used when the flap pans over a portion of intact skin which is preferred left untouched rather than split by a bridging incision.
The choice of the type of subdermal flap to use depends on the relative orientation and position of the skin in excess to be transferred and the wound to be covered.
The axillary and inguinal skin folds can be used to create a wide range of subdermal skin flaps. These skin folds are attached in 4 places, 2 (medial and lateral) on the trunk and 2 (medial and lateral) on the limb. Any 3 of these can be severed for the flap to be created, remaining attached by the 4th one.
| Figure 1. Subdermal flaps | 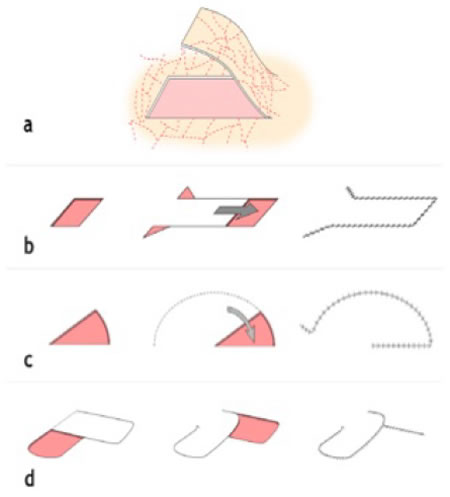
a: vascularisation; b: advancement flap; c: rotation flap; d: transposition flap |
|
| |