Jaundice may be caused by pre-hepatic, hepatic and post-hepatic disorders. The algorithm below (Figure 1) demonstrates the approach in identifying which of these groups of disorders is the most likely cause. Once the most likely group of disorders has been identified, consideration needs to be given as to what the most common diseases are in each group (Figure 2) and other basic clinical features need to be evaluated to direct the clinician to the most likely cause (Figure 3).
| Figure 1. Diagnostic approach to jaundice to differentiate pre-hepatic, hepatic and post-hepatic causes | 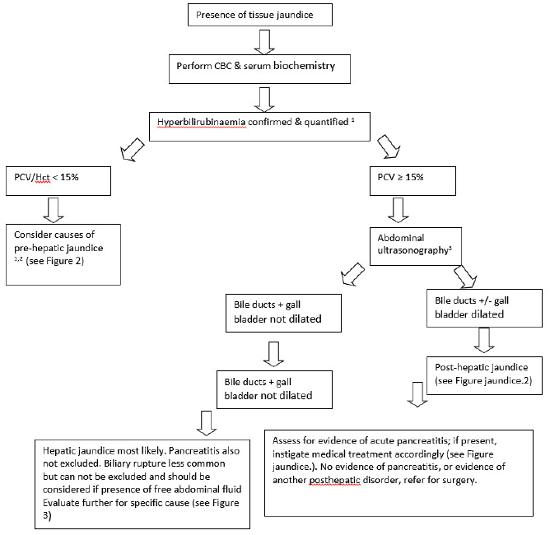
1. Tissue jaundice will only generally be evident when serum bilirubin exceeds approximately 50 μmol/l (reference range 0–15 μmol/l). The degree of hyperbilirubinaemia is also important in interpretation. There are no hard and fast rules but, generally, with pre-hepatic jaundice serum bilirubin is rarely above 50–100 μmol/l. FIP, pancreatitis, amyloidosis and sepsis also rarely result in serum bilirubin concentrations >100 μmol/l. When serum bilirubin is > 200 μmol/l, this is most often caused by either hepatic lipidosis or post-hepatic obstruction, which may be a surgical emergency. Hepatic lipidosis may frequently result in serum bilirubin concentrations > 200–300 μmol/l, but generally the higher the serum bilirubin, the more likely that complete post-hepatic biliary obstruction is present.
2. Haemolysis needs to be acute and severe (typically PCV < 13%) to cause clinically evident jaundice, and caution should therefore be taken in over-interpreting a mild anaemia to be the cause of jaundice. Cats will frequently have mild to moderate anaemia associated with chronic or inflammatory disease in hepatic and post-hepatic disorders. The degree of anaemia needs to be carefully interpreted with the degree of hyperbilirubinaemia, together with other clinicopathological features.
3. If serum bilirubin is > 100 μmol/l, abdominal ultrasonography is critical in identifying whether extrahepatic biliary duct obstruction is present. Where abdominal ultrasonography is not immediately available, if serum bilirubin is < 100 μmol/l, other clinical features (Figure jaundice.3) can be evaluated first to assist in identifying the most likely cause. Detecting early or partial extrahepatic biliary duct obstruction may require expertise in ultrasonography and referral may need to be considered. For the practitioner, the priority is to know if the case is a surgical emergency, and in this case the bilirubin is frequently > 250 μmol/l and the gall bladder and common bile duct grossly distended. |
|
| |
| Figure 2 | 
|
|
| |
Figure 3. Most common diagnoses associated with specific clinical features
|
Clinical features
|
Most common diagnoses
|
|
Age
|
|
|
Young
|
FIP (typically 6 month–3 years), lymphocytic cholangitis (typically 1–5 years)
|
|
Young to middle-aged (typically 2–8 years)
|
Pancreatitis, neutrophilic cholangitis, hepatic lipidosis
|
|
Middle-aged to older (typically > 8 years)
|
Neutrophilic cholangitis, hepatic lipidosis, pancreatitis, neoplasia
|
|
Breed
|
|
|
Siamese/Oriental
|
FIP, amyloidosis
|
|
Persian
|
FIP, lymphocytic cholangitis
|
|
Pedigree
|
FIP
|
|
History/clinical signs
|
|
|
Overweight with recent weight loss
|
Hepatic lipidosis
|
|
Weight loss despite a good appetite
|
Lymphocytic cholangitis
|
|
Any current medications
|
Consider possible hepatotoxicity
|
|
Abdominal pain
|
Pancreatitis, acute neutrophilic cholangitis, cholecystitis
|
|
Physical examination
|
|
|
Pyrexia
|
FIP, neutrophilic cholangitis, sepsis
|
|
Hepatomegaly
|
Lymphocytic cholangitis, hepatic lipidosis, neoplasia
|
|
Ascites
|
Lymphocytic cholangitis, FIP, neoplasia, haemoabdomen associated with amyloidosis
|
|
Respiratory compromise
|
Could be associated with pleural effusion - FIP, neoplasia
|
|
Laboratory test results
|
|
|
Anaemia
|
Haemolysis, anaemia of chronic inflammatory disease
|
|
Neutrophilia
|
FIP, sepsis, neutrophilic cholangitis, pancreatitis
|
|
Left shift/toxic neutrophils
|
Acute neutrophilic cholangitis, sepsis
|
|
More marked increase in ALT compared to ALP
|
Hepatotoxicity, amyloidosis, hepatic neoplasia
|
|
Mild hyperbilirubinaemia with normal ALT and ALP
|
FIP, pancreatitis
|
|
More marked increase in ALP compared to ALT
|
Post-hepatic jaundice, cholangitis, hepatic lipidosis
|
|
Extremely elevated ALP with only mildly elevated GGT
|
Hepatic lipidosis
|
|
Marked hyperglobulinaemia
|
Lymphocytic cholangitis, FIP
|
|
Hypocalcaemia
|
Pancreatitis, sepsis
|
|
Diagnostic imaging
|
|
|
Radiopaque area in gall bladder
|
Cholelithiasis
|
|
Hepatomegaly
|
Lymphocytic cholangitis, hepatic lipidosis, neoplasia
|
|
Ascites
|
Lymphocytic cholangitis, FIP, neoplasia, haemoabdomen associated with amyloidosis, biliary tract rupture (uncommon)
|
|
Thickened gall bladder wall/sludge in gall bladder
|
Cholecystitis/acute neutrophilic cholangitis
|
|
Marked hyperechoic hepatic parenchyma
|
Hepatic lipidosis, lymphoma (less common)
|
Other clinical features are also important to take into consideration in interpretation of results, including:
 Cat's age and breed
Cat's age and breed
 Other clinical signs present (e.g., vomiting, abdominal pain, tachypnoea/dyspnoea, inappetence, polyphagia, weight loss) and duration of clinical signs
Other clinical signs present (e.g., vomiting, abdominal pain, tachypnoea/dyspnoea, inappetence, polyphagia, weight loss) and duration of clinical signs
 Physical examination findings (e.g., body condition score, presence of pyrexia, hepatomegaly, ascites, abnormal/reduced lung sounds, cardiovascular compromise)
Physical examination findings (e.g., body condition score, presence of pyrexia, hepatomegaly, ascites, abnormal/reduced lung sounds, cardiovascular compromise)
 Other laboratory findings (e.g., neutrophilia, presence of left shift/toxic neutrophils, anaemia, degree of ALT/ALP/GGT elevation, hyperglobulinaemia)
Other laboratory findings (e.g., neutrophilia, presence of left shift/toxic neutrophils, anaemia, degree of ALT/ALP/GGT elevation, hyperglobulinaemia)
 Other diagnostic imaging findings (e.g., radio-opaque choleliths, hepatomegaly, ascites, mesenteric lymphadenopathy, gall bladder wall thickening/sludge, hyperechoic hepatic parenchyma)
Other diagnostic imaging findings (e.g., radio-opaque choleliths, hepatomegaly, ascites, mesenteric lymphadenopathy, gall bladder wall thickening/sludge, hyperechoic hepatic parenchyma)
Empirical Treatment Pending Investigations/Results
Intravenous Fluid Therapy
0.9% NaCl, usually supplemented with potassium chloride (KCl) depending on serum potassium concentration but if potassium cannot be measured, supplement with 20 mmol/l KCl.
Two–4 ml/kg/h usually an appropriate fluid rate depending on degree of dehydration.
Vitamin K
If clotting times cannot be easily assessed, it is worth treating with vitamin K in case of vitamin K dependent coagulopathy, especially if there is the possibility of surgical intervention.
Assisted Feeding
If inappetent, and vomiting controlled, consider placing naso-oesophageal feeding tube for short-term assisted feeding.
Analgesia
If abdominal pain present, or if neutrophilic cholangitis or pancreatitis suspected.
Buprenorphine 0.01 mg/kg sublingual or slow IV q 8 h.
Anti-Emetics
If vomiting/nausea is a feature: Maropitant (1 mg/kg SQ q 24 h up to 5 consecutive days) and/or metoclopramide constant rate infusion.
Antibiotics
If acute neutrophilic cholangitis or sepsis suspected, based on clinical findings.
Broad spectrum (e.g., amoxicillin/clavulanate, cephalexin) initially administered parenterally.
When to Refer
Given the large number of causes of jaundice, the difficulty in reaching a definitive diagnosis without accurate biliary ultrasonography and hepatic biopsy, and the intensive treatment required for many of these disorders, consideration should be given to referral of any jaundiced cat. In particular, referral is appropriate if post-hepatic obstruction is suspected, if liver biopsy is required, if the diagnosis is uncertain or if intensive treatment (e.g., in hepatic lipidosis) is required.