K. Borgeat
Arterial Thromboembolism: What We Know
Arterial thromboembolism (ATE) is a condition associated with high morbidity and mortality in cats, most commonly with an acute and distressing presentation. For clinical purposes, it is often defined as thromboembolism to ≥ 1 limb. In most cases, the thrombus originates in the left side of the heart; feline ATE is most commonly associated with cardiomyopathy, although cardiac disease is not present in all affected cats. Although pulmonary thromboembolism also involves arterial occlusion, it usually is classified as a separate syndrome. Presenting signs of limb ATE are easily recognized. Loss of peripheral pulses, tissue pallor, lower motor neuron signs and cool extremities in the presence of neuromuscular pain provide a highly suggestive clinical picture. Smith et al. reported that 1/175 (0.6%) of their hospital feline population presented with ATE, a similar prevalence to 1/142 cats (0.7%) reported by Buchanan et al. from a different centre, almost 40 years earlier. These data were obtained from cats treated in referral practice and do not necessarily represent the general feline population. Borgeat et al. (2014) published findings in 250 cats with ATE in general practice, and the prevalence was 0.26%—less than half that reported from referral centres.
It is widely acknowledged that ATE has a poor prognosis, although no prospective studies have reported the outcome of cats presenting with a first episode of acute clinical signs. Several retrospective studies suggest that euthanasia at presentation is common and < 50% patients survive to discharge. Smith et al. reported that hypothermia, ≥ 2 affected limbs, absence of motor function, hyperphosphataemia and bradycardia were associated with a decreased rate of survival to discharge. Moore et al. also reported that hypothermia and ≥ 2 affected limbs were associated with death or euthanasia before discharge. It has been suggested that cats in congestive heart failure (CHF) have a shorter survival time after discharge (Smith et al. 2003). Among cats discharged from the clinic, recurrence of ATE is common.
In first opinion clinics, rectal temperature is also vital to assess at presentation: lower rectal temperature was crucial in predicting death at 24 h and before 7 days of an ATE episode (Borgeat et al. 2014). Interestingly, this retrospective study also reported that treatment with an antiplatelet agent (aspirin, clopidogrel, or both drugs) was associated with an increased likelihood of survival to 7 days. We believe that immediate analgesia and antiplatelet agents are the standard of care for cats with an ATE, and if rectal temperature is particularly low or pain cannot be controlled, we recommend euthanasia as a viable treatment option.
Of cats treated for ATE in general practice, survival to 7 days is estimated at 55%. Of those cats alive at 1 week after an acute ATE episode, 1-year survival was 20%. Despite mortality being high in this population, and recurrence of ATE approaching 80%, quality of life in between episodes is often good and longer-term survival is possible (Borgeat et al. 2012).
| Approach to treatment of ATE | 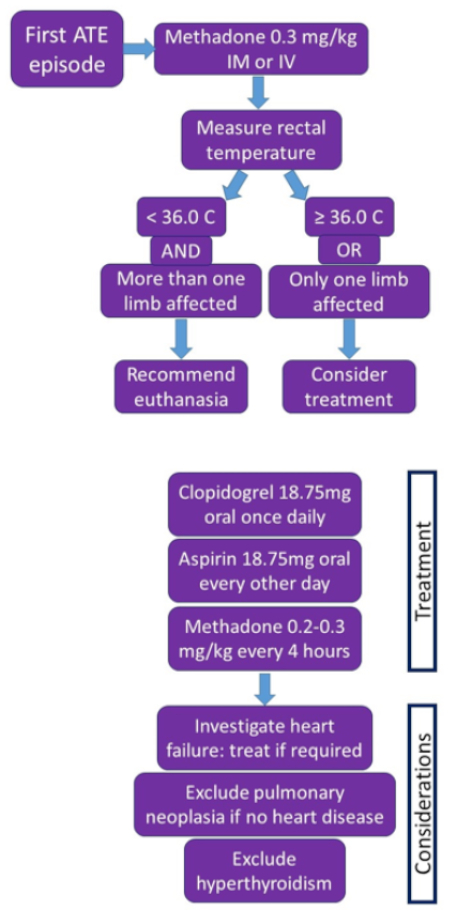
|
|
| |
Why We Should Choose Clopidogrel Over Aspirin: The FAT CAT Study (Hogan et al. 2015)
Over several years, the feline arterial thromboembolism clopidogrel vs. aspirin trial, or FAT CAT study, recruited cats that were at risk of ATE. Because identifying risk is difficult, the researchers recruited cats that had suffered an episode of ATE and had survived for 3 months (so they were known to have stable disease and would not die or be euthanised as a result of acute consequences of the first ATE). Cats were randomised to receive either clopidogrel (ADP receptor antagonist) 18.75 mg once daily or aspirin (thromboxane receptor antagonist) 18.75 mg every third day. Cats were followed until either ATE recurrence, or death because of heart disease.
This study showed that cats receiving clopidogrel lived for an average of 442 days before ATE recurrence, compared to an interval of 192 days observed in the aspirin group. Despite its more frequent dosing interval (and apparently a bitter taste to around 10–20% of cats), the drug is highly effective at preventing ATE, so should be considered the standard of care in cats with heart disease at risk of ATE—i.e., those with LA dilation or poor atrial function.
References
1. Borgeat K, Wright J, Garrod O, et al. Arterial thromboembolism in 250 cats in general practice: 2004–2012. J Vet Intern Med. 2012;28:102–108.
2. Hogan DF, Fox PR, Jacob K, et al. Secondary prevention of cardiogenic arterial thromboembolism in the cat: the double-blinded, randomized, positive-controlled feline arterial thromboembolism; clopidogrel vs. aspirin trial (FAT CAT). J Vet Cardiol. 2015;17:S306–S317.
3. Payne JR, Borgeat L, Brodbelt DC, et al. Risk factors associated with sudden death vs. congestive heart failure or arterial thromboembolism in cats with hypertrophic cardiomyopathy. J Vet Cardiol. 2015;17:S.318–S.328.
4. Smith SA, Tobias AH, Jacob KA, Fine DM, Grumbles PL. Arterial thromboembolism in cats: acute crisis in 127 cases (1992–2001) and long-term management with low-dose aspirin in 24 cases. J Vet Intern Med. 2003;17:73–83.
5. Buchanan JW, Baker GJ, Hill JD. Aortic embolism in cats: prevalence, surgical treatment and electrocardiography. Vet Rec. 1966;79:496–505.
6. Laste NJ, Harpster NK. A retrospective study of 100 cases of feline distal aortic thromboembolism: 1977–1993. J Am Anim Hosp Assoc. 1995;31:492–500.
7. Schoeman JP. Feline distal aortic thromboembolism: a review of 44 cases (1990–1998). J Feline Med Surg. 1999;1:221–231.
8. Moore KE, Morris N, Dhupa N, Murtaugh RJ, Rush JE. Retrospective study of streptokinase administration in 46 cats with arterial thromboembolism. J Vet Emerg Crit Care. 2000;10:13.
9. Rush JE, Freeman LM, Fenollosa NK, Brown DJ. Population and survival characteristics of cats with hypertrophic cardiomyopathy: 260 cases (1990–1999). J Am Vet Med Assoc. 2002;220:202–207.