L. Findji
Laryngeal paralysis (LP) is a common cause of upper airway obstruction resulting from a dysfunction of the recurrent laryngeal nerve(s) resulting in paresis progressing to paralysis of all intrinsic laryngeal muscles, except for the cricothyroid muscle. It is most frequently an acquired disease affecting older dogs of large breeds, being an early sign of a general polyneuropathy.
The diagnosis of LP is essentially clinical. Early clinical signs include a change in phonation, inspiratory stridor and exercise intolerance. Gagging, coughing and retching, as well as vomiting/regurgitations and dysphagia may also be reported. Later in the course of the disease, dyspnoea, respiratory distress, cyanosis and syncopes may be observed. A suspected LP can be confirmed in several ways. Although other diagnostic tests have been reported, the most common is direct or videoscopic transoral observation of the larynx under light general anaesthesia. Diagnostic tests aiming at screening for concurrent diseases are also carried out: haematology, blood biochemistry, thyroid function exploration and acetylcholine receptor antibody titres (myasthenia gravis). Thoracic X-rays are also recommended to rule out pre-existing aspiration pneumonia and other concurrent diseases which could affect the prognosis, such as megaoesophagus.
The larynx mainly consists of 4 cartilages: the epiglottic, arytenoid (paired), thyroid and cricoid cartilages. These cartilages are united by joints (fibrous or synovial) and muscles. The combined actions of intrinsic laryngeal muscles on these cartilages modify the size, shape and position of the glottis, rostral opening to the (infraglottic) laryngeal lumen and trachea. All intrinsic laryngeal muscles except the cricothyroid, which is innervated by the cranial laryngeal nerve, are innervated by the caudal laryngeal nerve, terminal segment of the recurrent laryngeal nerve (RLN). The RLN originates in the thorax from the vagus nerve and courses cranially up to the larynx, dorsolaterally to the trachea.
Currently, only two types of techniques are commonly used for definitive surgical correction of LP: arytenoid lateralisation techniques and partial laryngectomy techniques. Unilateral arytenoid lateralisation (UAL) is the most commonly used technique,1 as it appeared associated with fewer complications than bilateral arytenoid lateralisation and partial laryngectomy2. It has the author's preference and will be the only treatment described here.
For a lateral approach, the animal is placed in lateral recumbency and a cushion can be placed under its neck to elevate the laryngeal area towards the surgeon. The skin is incised over the larynx, ventrally and parallel to the external jugular vein. The subcutaneous connective tissues and cutaneous muscles overlying the larynx are reflected by a combination of blunt and sharp dissection. The thyropharyngeus and cricopharyngeus muscles are then visible and the dorsal border of the thyroid cartilage lamina is palpable through them. Rather than transecting the thyropharyngeus muscle transversely, we prefer to separate its fibres by blunt dissection over the middle of the dorsal edge of the thyroid cartilage. The separated fibres are then retracted with blunt Gelpi retractors, which provides enough exposure of the thyroid cartilage lamina, covered by a fascial membrane. This laryngeal fascial membrane is incised and the laryngeal mucosa is detached from the medial aspect of the lamina of the thyroid cartilage. This is done by combination of scalpel incision over the dorsal edge of the thyroid cartilage and blunt dissection with a Freer periosteal elevator or cotton-buds. Dissection is performed delicately to avoid perforation of the laryngeal mucosa and penetration into the lumen of the larynx. In addition, dissection is limited cranially to avoid damage to the cranial laryngeal nerve, which carries fibres supplying the sensory information from laryngeal mucosa. Preserving these fibres may minimise the incidence of postoperative aspiration of food. The lamina of the thyroid cartilage is retracted laterally using one stay suture. Disarticulation of the cricothyroid joint is not necessary for sufficient exposure of the arytenoid cartilage. The muscular process of the arytenoid is palpated and the cricoarytenoideus dorsalis is transected just caudally to it. The caudal part of the cricoarytenoid joint capsule is incised, but its rostral part is left intact to limit the later abduction of the arytenoid. The author does not section the interarytenoid structures (interarytenoid "band") in order to minimise the laryngeal disruption and decrease the risk of mucosal perforation. One or two "simple interrupted" sutures are placed between the dorsolateral aspect of the cricoid cartilage and the muscular process of the arytenoid cartilage (Figure 1). Placement of the suture through the cricoid cartilage is done in a caudo-rostral direction. The caudal border of the cricoid cartilage is only palpated: dissection aiming at visualising it is unnecessary. Alternatively, a thyroarytenoid suture may be used by placing the suture through the caudo-dorsal portion of the lamina of the thyroid cartilage. In the arytenoid cartilage, the suture is passed medio-laterally. Along the rostro-caudal axis, both sutures are placed in the middle of the arytenoid articular surface. Along the ventro-dorsal axis, the two sutures are evenly spaced, at the ventral and dorsal third of the arytenoid articular surface. The sutures are tied but not excessively tightened, as low-tension sutures have proved equally efficient in decreasing airway resistance and decrease the portion of the rima glottidis remaining uncovered when the epiglottis is closed. In doubt, an assistant may extubate the animal and control transorally that the arytenoid abduction is satisfactory. The lamina of the thyroid cartilage is released, the thyropharyngeus muscle fibres are apposed in a cruciate pattern and the wound is closed routinely. If it has not been assessed intraoperatively, the arytenoid abduction is controlled postoperatively by transoral visualisation.
| Figure 1. Schematic representation of the placement of a cricoarytenoid suture without disruption of the cricothyroid joint | 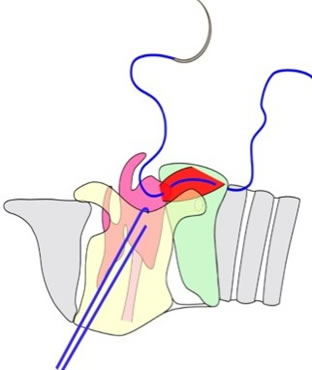
|
|
| |
In dogs without clinical signs of concurrent disease, the prognosis after UAL is fair. In a recent study, the 1-, 2-, 3-, and 4-year survival rates were 93.6%, 89.1%, 84.4%, and 75.2%, respectively.3 However, as described above, most affected animals suffer from generalised neuromuscular disease, which is the main determinant of their long-term prognosis. In one study, 6 of 11 dogs with acquired LP died or were euthanized within 15 months of diagnosis as a result of progression of clinical signs associated with their polyneuropathy.4
Aspiration pneumonia is the most commonly described complication after surgical treatment for LP, being a greater risk when a megaoesophagus is present.3 After unilateral arytenoid lateralisation, it has been reported to occur in 8 to 32% of cases. Aspiration pneumonia can occur months to years after surgery and operated dogs remain at risk for the remainder of their lives, but it seems that the risk decreases over time. Perioperative administration of metoclopramide was initially thought to lower the risk of aspiration pneumonia,5 but this was not confirmed in more recent studies3,6.
References
1. Monnet E. Surgical treatment of laryngeal paralysis. Vet Clin North Am Small Anim Pract. 2016;46:709–717.
2. MacPhail CM, Monnet E. Outcome of and postoperative complications in dogs undergoing surgical treatment of laryngeal paralysis: 140 cases (1985–1998). J Am Vet Med Assoc. 2001;218:1949–1956.
3. Wilson D, Monnet E. Risk factors for the development of aspiration pneumonia after unilateral arytenoid lateralization in dogs with laryngeal paralysis: 232 cases (1987–2012). J Am Vet Med Assoc. 2016;248:188–194.
4. Thieman KM, Krahwinkel DJ, Sims MH, Shelton GD. Histopathological confirmation of polyneuropathy in 11 dogs with laryngeal paralysis. J Am Anim Hosp Assoc. 2010;46:161–167.
5. Greenberg MJ, Reems MR, Monnet E. Use of perioperative metoclopramide in dogs undergoing surgical treatment of laryngeal paralysis: 43 cases (1999–2006). Vet Surg. 2007;36:E11.
6. Milovancev M, Townsend K, Spina J, Hurley C, Ralphs SC, Trumpatori B, et al. Effect of metoclopramide on the incidence of early postoperative aspiration pneumonia in dogs with acquired idiopathic laryngeal paralysis. Vet Surg. 2016;45:577–581.